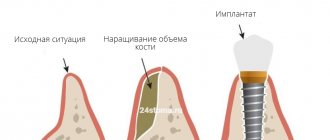
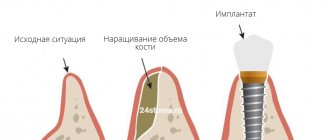
The roots of our teeth are located in the bone tissue of the jaw. Due to the fact that during chewing food the bone receives load from the teeth, it functions fully and is saturated with nutrients. But as soon as the tooth is removed, an empty space forms in its place - the bone cells grow quite slowly and do not have time to fill this space. As a result, the bone decreases in size, besides, metabolic processes are disrupted and cells stop receiving oxygen and nutrients. The bone atrophies.
Bone atrophy is a big problem when many teeth are missing. Indeed, in this case, not only aesthetic and psychological problems arise (facial skin sags, wrinkles appear near the lips, cheeks sag, lips become thinner and sink into the oral cavity), but also functional ones - after all, it is unlikely that you will be able to eat fully and efficiently without teeth .
Directed bone tissue regeneration is a surgical operation, the purpose of which is to restore the volume of the jaw bone, that is, to increase it to the previous size established by nature. This operation is mainly carried out as a preparatory stage before dental implantation - after all, in order to implant and securely fasten implants (artificial metal roots), a sufficient volume of strong bone is required. Sometimes it can be carried out together with the installation of implants.
Special offers!
Bone grafting, open sinus lift - RUB 35,000. Closed sinus lift (area of 1 tooth, excluding the cost of bone substitute) - RUB 10,000. Guided regeneration of bone tissue (area 1 tooth) - RUB 10,000. Guided bone regeneration (GBR) - RUB 35,000.
Materials for bone tissue augmentation
The word “regeneration” itself translated from Latin means “rebirth” or “renewal”. The operation is performed surgically and its essence boils down to replanting bone material in an area where the volume of the jaw bone is insufficient.
Various materials can be used for bone tissue regeneration:
- the patient's own bone: the most preferable option, since in this case 100% result of engraftment of the material is achieved. A piece of bone is usually borrowed from the chin area, the angle of the lower jaw (where the outermost wisdom teeth are located) or the hip area. The obvious disadvantage is that it is often necessary to perform two surgical interventions simultaneously,
- artificial synthetic materials: developed in laboratory conditions. A fairly common option, today it is used everywhere, in most cases as an additional material when grafting the patient’s own bone. Has good survival rate,
- related bone: This is typically cleaned cadaveric bone from another person that is kept in a sterile jar. It also takes root well and does not require additional surgical intervention.
- animal bone: the material can be presented in the form of bone blocks or in the form of shavings. It takes root well and is almost not rejected.
Bone regeneration: how is it done?
The operation lasts 1-2 hours, depending on the volume and complexity of the work. After 3-4 months, when the implanted piece has fused with the natural bone, it will be possible to proceed to the installation of implants. In some cases, it may take longer to engraft, depending on the individual characteristics of the organism. The technology for bone tissue regeneration is as follows:
- anesthesia is administered, in some cases, if serious surgery is required, it is possible to perform the operation under anesthesia,
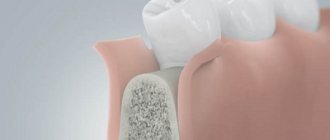
- access to the bone is created: a piece of gum is cut and peeled off, with the help of protective membranes, which dissolve on their own over time, a cavity is formed to be filled with bone chips,
- bone material is introduced: the cavity is filled with artificial or natural bone material. After 2-4 months, the natural bone cells will penetrate deep into the implanted material, and it will turn into its own bone tissue - then implantation can begin. On top of the new bone is covered with a protective membrane, which will protect against pressure from the gums,
- The gum is sutured - sutures are fixed on the mucous membrane, which are removed on average after a week.
Expert opinion
Emir Romanovich Omerelli
Maxillofacial surgeon, implantologist
Experience: more than 13 years
If, based on the results of the examination, the doctor diagnoses a lack of bone tissue, it is necessary to increase its volume before implantation. Placing implants in low or narrow bone carries serious risks. The bone may fracture or the implant itself may fall out after a short period of use. To prevent this from happening, before classical implantation of the upper teeth, it is necessary to carry out a sinus lift, and for the lower teeth, extension through osteoplasty. The only exception is the basal protocol, according to which implants can be installed without bone grafting and without risks.
If the bone tissue is not wide enough, that is, it is very thin, the operation can be performed by splitting the alveolar ridge: first the gums are exfoliated, then the bone is cut along the length and artificial or natural bone material is placed inside.
Also, the problem of narrow bone tissue is solved by transplanting a bone block borrowed from another bone of the patient himself. To do this, a piece of bone is placed under the gum, fixed with special screws, sprinkled with bone chips around it, covered with a barrier membrane and gum - the mucous membrane is sutured. This option is more preferable, since in most cases the own bone survives.
Bone tissue augmentation surgery, depending on the indications, can be performed simultaneously with the installation of classical implants without their subsequent loading. That is, the artificial roots are fixed in the bone, but are covered by the gum - the dentures will be fixed in 3-4 months. In order for classical implants to take root in the bone, it is necessary to ensure their rest and relieve any pressure.
Complications after bone tissue regeneration
The operation of bone tissue augmentation is considered one of the safest in dentistry, complex, but if carried out correctly, without any unpleasant consequences. In the first days after the operation, it becomes clear whether the block will take root or the operation will have to be performed again. Among the unpleasant sensations are slight tissue swelling and pain in the area where the bone block was taken and the site where it was transplanted. But after 2-4 days, all unpleasant sensations go away on their own.
After bone augmentation
After the bone regeneration procedure, the patient must take precautions: be sure to take medications prescribed by the doctor to quickly restore the body, and do not ignore painkillers. You should refrain from eating food for 2-3 hours after surgery; afterwards it should be warm, but not too cold or hot. It is recommended to chew foods on the side opposite the surgical procedure. In addition, it is necessary to give up physical activity for a while and provide the body with rest for a couple of days after the operation. Do not forget to visit your doctor for a preventive examination and monitor the results of treatment.
Other jobs
Sources of regeneration
Restoration of bone integrity occurs through the proliferation of cells of the osteogenic layer of the periosteum, endosteum, insufficiently differentiated pluripotent cells of the bone marrow, as well as due to metaplasia of giaraosseous tissues.
Modern ideas about the processes of bone tissue regeneration combine the concepts of neoplastic and metaplastic theories. Preosteogenic cells are considered osteoblasts, fibroblasts, osteocytes, pericytes, histiocytes, lymphoid, fat and endothelial cells, cells of the myeloid and erythrocyte series.
During the fusion of broken bones, a staged pattern of reparative osteogenesis has been established, which is conditional. The division into stages is not of fundamental importance, since they overlap in dynamics.
Even with ideal reposition and fixation of fragments, differentiation of various cells occurs simultaneously, and therefore the stages of the reparative process are difficult to distinguish. But to choose the optimal treatment tactics for patients, you need to have an idea of the patterns of reparative osteogenesis.
Examples of work “Before” and “After”
Restoration of all teeth on the upper and lower jaw - basal implantation
Case: partial absence of teeth on the upper and lower jaw, complicated by severe periodontitis (tooth mobility).
Complex one-stage implantation of the lower jaw
Case: there was a loose bridge of 4 front teeth on the lower jaw; after diagnosis, removal of the remaining teeth and coplex basal implantation were prescribed.
Restoration of all teeth using basal implantation method (March 2012)
Case: partial adentia, exposed roots of natural teeth, periodontitis, increased tooth mobility, severe atrophy of bone tissue in some places beyond the possible norms for classical dental implantation.
Restoration of anterior teeth using basal implantation method (April 2012)
Case: partial absence of front teeth and destruction of supporting teeth under the prosthesis, the relief of the gums and interdental papillae is disturbed.
Bone Regeneration: Basics
Reparative regeneration is the restoration of damaged or lost tissue. The degree and quality of the regenerative process in different tissues is different. The higher the differentiation of the tissue (nervous, muscle), the less ability it has to restore its structure. Therefore, anatomical restoration of the damaged area occurs by replacing the defect with connective tissue - a scar. Damaged bone tissue is able to go through a number of stages of the reparative process and restore its anatomical shape, histological structure and functional suitability.
A bone fracture is accompanied by damage to adjacent soft tissues and causes a stressful situation, which is accompanied by local and general reactions of the body. During the process of bone tissue restoration, complex general and local biological and biochemical changes occur, which depend on the blood supply to the bone, the age of the patient, the general condition of the body, and the quality of treatment.
Can it be done simultaneously with implantation?
Two operations are combined into one if the following conditions are met:
- the shape of the defect allows you to correctly install the artificial root in any of the planes;
- when installed, the implant is located within the bone contour (does not go beyond the tangent drawn to the bone line);
- eliminate a horizontal (not vertical) defect.
The implanted implant can become a barrier to the growth of blood vessels and inhibit the formation of new bone. If the implant protrudes beyond the contour of the bone tissue, the risk of developing fibrous tissue with inclusions of the implanted material cannot be ruled out.
What is Guided Bone Regeneration
Guided bone regeneration is an operation to compensate for the lack of bone tissue with a substitute, which is secured with a barrier membrane. After the procedure, a framework is formed around the transplant (it is formed by vessels and osteocyte cells that produce new tissue). Natural bone is gradually replacing artificial material.
Extensions using the NDT method are carried out according to classical parameters:
- thickness of the vestibular bone wall (at the cheek) - up to 2-2.5 mm;
- bone thickness between the implant and the root of the adjacent unit - up to 2.5-3 mm;
- The thickness of the bone wall between two titanium roots is up to 3 mm.
Types of membranes
The membrane technique used by the surgeon is needed to isolate the space from fibrous tissue - creating conditions for normal tissue regeneration. There are several requirements for membranes:
- biological compatibility;
- strength;
- prevention of migration of epithelial cells;
- corresponding resorption period.
In practice, two types of membranes are used:
- Resorbable.
They dissolve on their own 6-24 weeks after extension. Membranes are used for small defects (when you need to build up no more than 2 mm) - they do not hold their shape as well as the next type. - Non-resorbable.
They do not dissolve - they are eliminated several months after surgery.
To quickly fuse the artificial material with the jaw bone tissue, in some cases membranes from the patient’s blood plasma are used.
Indications
The operation allows you to increase the “necessary” volume for high-quality classical implantation, helps restore the functions of the jaw, and returns the gums to an attractive appearance.
The bone is built up “with reserve”, since after the operation the surface layers will be supplied with a small amount of oxygen due to their lower blood circulation. Therefore, the volume of inevitable tissue resorption is calculated.
In addition to implantation, indications for NRC are:
- rapid restoration of physiological parameters after tooth extraction;
- congenital or acquired defects of the bone around the teeth;
- prevention of tooth displacement, loosening, and loss due to periodontal tissue diseases.
Why does atrophy occur?
The effect of low frequency electrical stimulation on bone tissue regeneration
1.Clinic premorbid and emergency conditions FKU “MONKS” them. PV Mandryka MO, 121002 Moscow, Silver lane, 4. 2.FSBI research Institute of General pathology and pathophysiology, 125315 Moscow, the Baltic St.8. 3.FSBI Institute of biology of development. NK Koltsov Academy of Sciences, 119334, Moscow, Vavilov St, 26. 4.LLC “Medical center HuanDi”
The study was performed on 30 male rats of Wistar line (weight 330 – 360 g, age 3.5 months). In an experimental model of damage to the femur bone in the hip joint studied the effect of low frequency electrical stimulation of the damaged area on the rate of regeneration of bone. The animals were divided into two groups. Control (15 rats) and experienced (15 rats). In the experimental animals received stimulation of the injury site for 5 min daily for 7 days, 14 days and 21 days. Stimulation was carried out using a device “Osteon-1” generating a mixed signal of two voltage pulse of varying duty cycle, one of which is modulated to a higher frequency. Signals were not synchronized with respect to each other, unipolar with varying frequencies and amplitudes. The obtained results show the effectiveness of the electrical stimulation currents of low frequency in the restoration of bone tissue after damage. Morphological studies showed that electrical stimulation to accelerate the regeneration of damaged bone at all stages of the study (7,14,21 days), causes a more pronounced integration of newly formed bone with the old intact bone and promote the formation of more powerful periosteal calls in comparison with the control.
In most countries of the world, there is a significant decrease in mortality, as a result, an increase in life expectancy and, accordingly, an aging population [1]. However, improving health care does not mean improving the quality of life, both for an individual and for society as a whole. [2] . Unfortunately, the progress made in increasing life expectancy has not been matched by progress in reducing disability in older people.
It should be emphasized that the number of older people around the world is rapidly increasing. In particular, in the Russian Federation currently the share of old-age pensioners is 20.6% [3].
Osteoporosis is one of the most pressing problems of modern healthcare. In Russia, 14 million people over 50 years old suffer from osteoporosis. Another 20 million have osteopenia [4,5]. Osteoporosis ranks fourth in the frequency of disability after diseases of the cardiovascular system, diabetes and cancer.
According to WHO, about 75 million citizens of Europe, the USA and Japan suffer from this disease. Due to the aging population of Europe, by 2050 the number of osteoporotic fractures of the femoral neck is expected to increase from 500 thousand to 1 million cases annually [6. Osteoporosis is especially common in older women due to decreased levels of sex hormones. In addition to fractures, there is also a steady increase in degenerative diseases of the joints (osteoarthrosis, osteoporosis, aseptic necrosis). Joint diseases are accompanied by chronic pain. Studies conducted in the USA have shown that women experiencing pain fall 1.66 times more often [7], and this, in most cases with osteoporosis, inevitably leads to bone fractures.
The general pathogenetic mechanism of this group of diseases is a violation of the structure of bone tissue, accompanied by a complex local or systemic disruption of the processes of bone remodeling.
All of the above indicates that the problem of treating bone remodeling disorders is relevant and, due to the increasing aging of the population, is becoming increasingly relevant.
The accumulated experience in drug treatment of degenerative diseases shows that none of the currently existing drugs can reliably restore the quantity and quality of bone tissue [8]. In addition, one should take into account the fact that elderly and old people, as a rule, have a number of comorbid conditions and, accordingly, there is forced polypharmacy. Therefore, in recent decades, an intensive search has been carried out for the possibility of using not pharmacological, but physical methods to stimulate osteogenesis: alternating electromagnetic fields of high and low frequencies, direct electric current, ultrasound, which have a number of advantages in their practical application [9-11]. The advantages of these methods of influence are: safety, the possibility of long-term multifactorial effects, and lack of addiction.
Experience in the treatment of necrosis of the femoral head has shown that external electrical signals can trigger a cellular response leading to reconstruction of the damaged bone [12-15].
Taking into account the results of numerous experimental and clinical studies indicating the effective effect of electrical stimulation on various body systems and, in particular, on reducing joint stiffness, muscle spasticity and suppressing pain after fractures, accelerating bone regeneration [9, 16-18], the Osteon device was developed -1" for effective restoration of bone tissue structure [13].
The purpose of this work is a histological study of the effectiveness of bone tissue restoration when stimulating damaged animal bones using the Osteon-1 device.
Methodology
The work was performed on 30 male Wistar rats (weight 330 – 360 g, age 3.5 months). The rats were kept under standard conditions, 5 animals per cage, with controlled temperature (24 oC) and lighting (for 12 hours) and with free access to water and food. The operation to simulate the injury was performed under general anesthesia. First, the animals were anesthetized with light ether anesthesia. For deeper anesthesia, chloral hydrate was used intraperitoneally at a dose of 300 mg/kg. Then the animal was fixed on the operating table, the hair in the left thigh area was trimmed, and the skin and muscle tissue was cut with a scalpel. The femur in the area of the hip joint was exposed, the femur was drilled to the medullary canal 8-10 mm distal to the hip joint using a miniature dental drill (bur diameter 0.8 mm). After bone damage, layer-by-layer suturing of soft tissues was performed. The animals were divided into two groups. Control (15 rats) and experimental (15 rats). In experimental animals, using the Osteon-1 device, stimulation of the injury area was performed for 5 minutes daily for 7 days. (op7), 14 days. (op14) and 21 days (op21). To do this, the animals were fixed on operating tables and a mixed signal of two pulse voltages of different duty cycles, one of which was modulated at a higher frequency, was supplied through surgical needles inserted under the skin. The signals were unsynchronized relative to each other, unipolar with varying frequencies and amplitudes. The cathode was located in the area of injury, the anode was placed distally on the same paw. Electrical stimulation was carried out under general anesthesia (chloral hydrate at a dose of 190-200 mg/kg, intraperitoneal).
Three groups of animals with trauma served as controls (k7, k14, k21); they were also placed on dissection tables; surgical needles were inserted into them, but stimulation was not carried out. In each experimental variant, 5 animals were used. The next day after the end of the study, the animals were removed from the experiment by cervical dislocation. Then the femurs of all 6 groups were removed, which were used for histological analysis and assessment of the severity of the pathological process and the process of osteogenesis.
Animal bones were fixed for 24 hours at room temperature in 10% formalin prepared in phosphate-buffered saline (PBS, 0.02 M, pH 7.6). They were decalcified in 5% trichloroacetic acid for 48 hours, then washed in PBS and frozen in isopentane at -400C. Next, sections with a thickness of 5 μm were prepared. The sections were dried at room temperature for 1 hour and stained with hematoxylin-eosin. For histological analysis, 100 to 200 serial sections of the femur were prepared from each animal in the transverse and longitudinal directions. Using an Olympus microscope (approx. 10x, ob. 4x). Microphotographs of bone tissue sections were taken. Morphometric analysis of bone tissue inside the wound channel (intermediary callus) was carried out using the ImageJ program [19]. The area of bone tissue measured on 3-5 sections from each animal was expressed as a % of the canal area. To determine the significance of differences between the experiment and the control, the nonparametric two-sided Mann-Whitney test (U-test) was used.