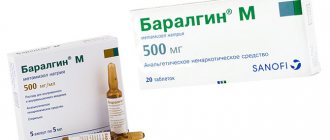
Characteristics of Ketorol
Ketorol belongs to the group of NSAIDs. The active ingredient is ketorolac. It has several dosage forms - film-coated tablets, solution for intramuscular and intravenous injections, gel for external use. It has analgesic, antipyretic and anti-inflammatory effects.
Ketorol is used to relieve acute pain, the cause and location of which may be different, including:
- periods after various medical procedures - orthopedic, gynecological, laparoscopic;
- injuries and burns;
- migraine, toothache;
- renal and hepatic colic;
- pain symptoms in sickle cell anemia;
- neuralgia, neuritis, pain syndrome with herpes zoster.
The drug is not used in the treatment of chronic pain.
Ketorol is contraindicated in case of individual intolerance to the substances included in its composition. The medicine is not prescribed for aspirin-induced asthma, peptic ulcer of the gastrointestinal tract, kidney disease, hemostasis, hemorrhagic stroke, congestive heart failure. This painkiller should not be used in the treatment of children and adolescents under 16 years of age.
If medical recommendations are not followed, side effects may develop, which are manifested by pain in the abdomen, dyspeptic symptoms, drowsiness, emotional anxiety, and allergies.
These drugs are considered the most powerful medications that can fight not only pain, but also inflammation and fever.
Characteristics of Ketanov
The active component of the drug is ketorolac. Available in the form of tablets and solution for injection. A strong analgesic effect is the main therapeutic property of the drug. It also fights inflammation and relieves fever.
Ketanov is considered the most powerful pain reliever among the drugs included in the NSAID group. Effectively combating pain of various origins, the drug is not a narcotic drug, i.e. it is not addictive.
Ketanov is used if it is necessary to quickly relieve pain of any location and origin:
- after operations and injuries;
- dental, muscle and postpartum pain;
- drug withdrawal;
- after dental procedures;
- renal or biliary colic;
- tumors;
- osteoarthritis, osteoarthritis, osteochondrosis;
- inflammation of the sciatic nerve.
We recommend reading: What is the difference between Ketonal and Ketonal Duo?
The drug has many contraindications for use:
- exacerbation of gastrointestinal ulcers;
- hemophilia and hypocoagulation;
- hemorrhagic stroke and diathesis;
- angioedema;
- aspirin asthma;
- spasms in the bronchi;
- chronic pain;
- pregnancy and lactation;
- age up to 16 years;
- intolerance to the components of the drug.
You should not take Ketanov without a doctor's prescription. This is a strong remedy and not recommended for everyday use.
You should not take Ketanov without a doctor’s prescription; it is a strong remedy and not recommended for everyday use.
Comparison of Ketorol and Ketanov
The drugs have both similarities and differences.
Similarities
Both drugs contain the same active ingredient, the same indications for use and contraindications. Ketanov and Ketorol belong to the same pharmacological group of non-steroidal anti-inflammatory drugs.
Both medications have the same release forms - for oral administration, injection and external use.
What is the difference?
Despite the great similarity, the drugs still differ from each other, for example by their manufacturers. Ketanov is produced by the Indian company S.K.Therapy S.A., and Ketorol is produced by another Indian company Dr. Reddy S Laboratories.
Which is stronger and more effective?
Ketanov is a stronger remedy. It is recommended to take it for complex injuries and burns. Under the influence of Ketorol, platelets stick together, so this medicine is considered more effective for wound healing.
When choosing a drug, you should also take into account contraindications, so you should carefully read the instructions. Ketanov has more of them.
Ketorol is less dangerous during pregnancy and breastfeeding. But you still shouldn’t use it without consulting a doctor.
Ketorol is less dangerous during pregnancy and breastfeeding, but you should still not use it without consulting a doctor.
Which is cheaper?
Ketorol price:
- tablets - from 40 rubles;
- solution - from 130 rubles;
- gel – from 230 rub.
Ketanov price:
- tablets - from 50 rubles;
- solution - from 100 rubles;
- gel – from 340 rub.;
- cream – from 310 rub.
Conditions for dispensing from pharmacies
Both drugs, available in gel or cream form, are over-the-counter products, and tablets and ampoules are available with a doctor's prescription.
We recommend reading: What to choose: Don powder or tablets?
How to take if your tooth hurts
Before answering questions about how long it takes for the drug to take effect and how long the effect lasts, it should be noted that both drugs effectively help cope with toothache of various etiologies. The effect in both cases occurs approximately 30-40 minutes after taking the tablet. How long does the product last? On average, the duration of the effect is 4-6 hours. As a rule, this time is enough to numb the inflamed area and alleviate your condition until you visit the dentist.
The effect of the tablets is 4-6 hours
Now let’s figure out how to take Ketanov and Ketorol tablets. There is no significant difference in the principles of taking these drugs. To relieve acute symptoms, it is enough to take one tablet. The maximum daily dosage is 5 tablets, but in most situations experts recommend taking 1-2 tablets per day with a sufficient amount of water. It is better to start eating half an hour after taking the painkiller.
Regarding how much “Ketanov” and “Ketorol” you can drink, we must immediately gently stipulate that these drugs are allowed to be taken for no longer than 7 days. If long-term therapy is necessary, the drugs are replaced with other non-steroidal anti-inflammatory drugs.
Which is better: Ketorol or Ketanov?
Even a doctor cannot accurately answer this question. When prescribing, many factors are taken into account, including the patient’s health status. It is not recommended to choose a medicine on your own.
For osteochondrosis
Ketorol has good anti-inflammatory properties. It copes with inflammation and pain quickly, so doctors often recommend it for osteochondrosis. But the contraindications of the drug should be taken into account. It is not suitable for some patients. Although the medicine is a better pain reliever, it is replaced with less effective medications.
For toothache
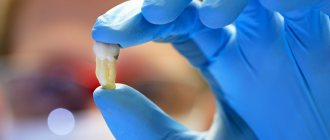
For toothache, Ketanov is considered a more suitable remedy. This is especially true for those patients who have had a diseased wisdom tooth removed, since their roots penetrate deep into the jaw. After removal, wounds remain that take a long time to heal, so the doctor recommends painkillers.
It is better to consult a doctor about what doses to take the medication.
Ketoprofen in the treatment of acute and chronic pain: review of literature data
Nonsteroidal anti-inflammatory drugs (NSAIDs) are the most important class of drugs used to relieve acute and control chronic pain in therapeutic practice. NSAIDs are distinguished by a combination of analgesic, anti-inflammatory and antipyretic effects, which provides them with an advantage over paracetamol and opioids [1–3].
Currently, nineteen different NSAIDs are registered in Russia. These are “international nonproprietary names,” i.e., chemical substances, and there are an order of magnitude more specific commercial drugs. Unfortunately, none of the modern NSAIDs can be considered ideal: if any drug has an advantage in one or another parameter, most likely, it also has serious disadvantages.
The main difference between different representatives of the NSAID group is their safety. Until recently, the main problem with these drugs was the development of complications from the gastrointestinal tract (GIT). All NSAIDs are cyclooxygenase (COX) 2 inhibitors, however, in addition to this action, they can inhibit the structurally similar enzyme COX-1. The work of the latter is necessary to maintain the protective potential of the gastrointestinal mucosa, so its blockade can lead to the development of dangerous gastrointestinal pathology - the so-called. NSAID gastropathy and NSAID enteropathy [4].
Selectivity for COX-2, and therefore the risk of developing gastrointestinal pathology, became the basis for dividing NSAIDs into two groups: “traditional” or non-selective (n-NSAIDs) and selective (s-NSAIDs). s-NSAIDs, so-called. “coxibs” were created in the late 90s of the last century as a safer alternative to “traditional” NSAIDs for the gastrointestinal tract. But, as it turned out, “coxibs” have a serious drawback: selective blockade of COX-2 can disrupt the balance of factors affecting blood clotting - the synthesis of thromboxane A2 and prostacyclin, which determines the prothrombotic effect. In patients with diseases of the cardiovascular system (CVS), this is fraught with an increased risk of thromboembolic complications, such as myocardial infarction (MI) and ischemic stroke [4].
This problem has renewed interest among practitioners in “traditional” NSAIDs, the use of which seemed to be associated with a significantly lower risk of cardiovascular (CV) complications.
But not all n-NSAIDs are safe against cardiovascular disease. Thus, the risk of CV complications when using the most popular representative of the “traditional” NSAIDs in Russia, diclofenac, is very high. This fact is shown by a meta-analysis of 25 population-based studies conducted in 18 independent populations and representing the individual risk of CV complications for different NSAIDs. The outcome measure was the incidence of myocardial infarction, which occurred in ~100,000 patients. Minimal risk of MI was shown for naproxen (odds ratio (OR) 1.06) and celecoxib (OR 1.12); for diclofenac this figure was 1.38 [5].
Another popular n-NSAID, ketoprofen, demonstrates a significantly lower risk of LE complications. This drug appeared in Europe in 1971 and quickly gained a reputation as an effective and reliable analgesic [6]. Over forty years of clinical use, it has not lost its significance. P. Sarzi-Puttini et al. emphasize this fact in a review with a very characteristic title: “Pain and ketoprofen: its role in clinical practice,” which was published in 2010. They point to a huge base of evidence of its effectiveness, a wide range of indications - in fact, all pathological processes accompanied by nociceptive pain, and a good reputation among doctors [7].
Interest in ketoprofen can be assessed by the increase in its prescriptions in European countries. Thus, M. Venegoni et al. showed that, against the backdrop of a small but clear decrease in overall sales of “prescription” NSAIDs in Italy for the period from 2006 to 2009. the popularity of ketoprofen has almost doubled (by 93%). If in 2006 263,897 residents of this country purchased ketoprofen, then in 2009 - already 508,699 [8].
Many experts associate the high analgesic potential of ketoprofen with the characteristics of its molecule. The lipophilicity and relatively small size of ketoprofen determine its ability to easily penetrate into inflamed tissue (for example, into the synovial cavity in arthritis), creating a high concentration [7, 9]. Great importance is attached to the diffusion of ketoprofen through the blood-brain barrier and its effect on the central structures of the pain system. Experimental data confirm the equilibrium concentration of the unbound fraction of ketoprofen in blood plasma and cerebrospinal fluid. Moreover, the central effect of this drug is associated not only with the blockade of COX-2, but also with other mechanisms, in particular, with its effect on the serotonergic antinociceptive system [10].
As noted above, the experience of using ketoprofen includes all diseases and pathological conditions for which the prescription of NSAIDs seems appropriate. Working with ketoprofen is facilitated by the availability of a full range of dosage forms: solution for intravenous (IV) and intramuscular (IM) administration, standard tablets, controlled-release capsules, forms for topical use, rectal suppositories.
Ketoprofen is a very successful remedy for urgent pain relief. In 2009, data from a Cochrane meta-analysis were published evaluating the results of a single dose of ketoprofen at a dose of 25–100 mg for acute postoperative pain. The material was based on data from 14 randomized controlled trials (RCTs) (968 patients treated with ketoprofen, 520 placebo), and the main evaluation criterion was a pain reduction > 50% for a period of 4 to 6 hours. The researchers used the NNT (number need to treat) index, which shows the number of patients who need to be treated to achieve a significant difference from placebo. This index was 2.4–3.3, which shows a fairly high effectiveness of the drug [11].
Data from a large-scale study (n = 338) were recently published, which examined the effect of a single intravenous administration of parecoxib 40 mg and ketoprofen 100 mg for the relief of acute renal colic. Ketoprofen, which acted as a comparison drug, was in no way inferior to the representative of “coxibs”: the reduction in pain (on a visual analogue scale - VAS) 30 minutes after injection was 35.2 ± 26.0 and 33.8 ± 24.6 mm [12 ].
The work of S. Karvonen et al. is an example of the successful use of ketoprofen in surgical practice. Here, ketoprofen at a dose of 300 mg/day was used in 60 patients who had undergone orthopedic surgery. The control group consisted of patients receiving placebo or paracetamol 4 g/day. The criterion for effectiveness, in addition to reducing the severity of pain, was the assessment of the “opioid-sparing” effect, which was determined by comparing the dose of fentanyl required for persistent analgesia. This effect was noted only in the ketoprofen group: the average dose of fentanyl was 22% less than in the placebo group and 28% less than in the paracetamol group [13].
Good results have been observed when using ketoprofen in dentistry. J. Olson N. et al. conducted a study in which 239 patients were prescribed a minimum dose of ketoprofen (25 mg), ibuprofen 400 mg or paracetamol 1000 mg after extraction of the 3rd molar; The “passive” control was placebo. The main evaluation method was to compare the number of patients who were completely free of pain 6 hours after tooth extraction. This result was achieved in almost all patients who received ketoprofen - 99%, in 96% of those who received ibuprofen and 88% - paracetamol (the difference is not significant). All active drugs were superior to placebo, which relieved pain in only one third of patients (33.6%). As can be seen, even a minimal dose of ketoprofen provides the same pronounced (and even slightly greater) pain relief as standard therapeutic doses of ibuprofen and paracetamol [14].
A successful demonstration of the benefits of ketoprofen was the work of I. Jokhio et al., who compared it with diclofenac in 180 patients experiencing severe pain (average VAS value ~70 mm) due to trauma or acute soft tissue pathology of a rheumatic nature. In this case, the so-called “stepped” therapy: on the first day, NSAIDs were administered as intramuscular injections and then orally. Accordingly, half of the patients received two injections of ketoprofen 100 mg each, and then took this drug 100 mg 2 times a day. The second group of patients received two injections of diclofenac 75 mg, and subsequently took it 50 mg 3 times a day orally. The course of treatment was 2 weeks. By the end of the observation period, ketoprofen showed better results (Fig. 1). At the same time, 72% of patients receiving ketoprofen rated its tolerability as “good or excellent”; Only 50% of patients gave this assessment to diclofenac [15].
One of the latest evidence of the high analgesic effectiveness of ketoprofen was the work of Italian scientists P. Sarzi-Puttini et al. — a meta-analysis of 13 RCTs (n = 898), which compared the effect of ketoprofen 50–200 mg/day with ibuprofen 600–1800 mg/day or diclofenac 75–100 mg/day in patients with various rheumatic diseases. Ketoprofen showed significant superiority over comparator drugs in 9 of 13 RCTs. Moreover, the likelihood of achieving a favorable effect when prescribing ketoprofen was almost 2 times higher (OR 0.459: 0.33–0.58, p = 0.000) [16].
Ketoprofen has proven to be an effective remedy for relieving a migraine attack. According to the results of a study by M. Dib et al., it was not inferior to zolmitriptan, a representative of the group of triptans, which are the most important pathogenetic agent for the treatment of this disease. In this study, 235 patients with migraine took a single dose of ketoprofen 75 or 150 mg or zolmitriptan. All groups showed almost the same result: after 2 hours, pain stopped in 62.6%, 61.6% and 66.8% of patients, respectively [17].
It should be noted that ketoprofen has good anti-inflammatory potential. The best model for assessing the anti-inflammatory effect of NSAIDs is the relief of gouty arthritis, in which severe pain is determined by an acute inflammatory response. Indomethacin, which has pronounced anti-inflammatory properties, has long been considered the “gold standard” for the treatment of this pathology. Ketoprofen, as shown by R. Altman et al., was successfully compared with this drug. In the study, 59 patients with acute gouty arthritis took ketoprofen 100 mg 3 times a day or indomethacin 50 mg 3 times a day for 7 days. Ketoprofen provided significant pain relief on the first day of treatment in 92% of patients; in the control group they were 91%. After a week of treatment, the attack was completely stopped in 24% and 22% of patients. As can be seen, ketoprofen was not inferior to indomethacin in effectiveness. But at the same time, it was clearly superior in safety - while taking indomethacin, any side effects were noted in 20% of patients, and in the ketoprofen group - only in 11% [18].
In addition to emergency pain relief, ketoprofen has proven to be effective for long-term pain control in chronic musculoskeletal diseases.
Important evidence of the merits of ketoprofen was a European prospective open study that included about 20 thousand patients with various rheumatic pathologies, mainly osteoarthritis (OA). After 1 month, more than 70% of patients taking ketoprofen at a dose of 200 mg/day reported good or excellent results; At the same time, gastrointestinal complications occurred in a total of 13.5%, and ulcers and bleeding in only 0.03% [19].
The work of M. Schattenkirchner et al. showed good tolerability of ketoprofen with long-term use. In their study, 823 patients with OA and rheumatoid arthritis received ketoprofen for a year. During treatment, complications from the gastrointestinal tract occurred in 28% of patients (only 1.7% were serious), and from the cardiovascular system - in 3.2%, which is relatively small, given the predominantly elderly age of the patients and severe comorbid background [20].
Successful results were obtained when using ketoprofen in patients with ankylosing spondylitis (AS). In AS, NSAIDs play the role of the main therapeutic agent to control the progression of the disease. In a study by M. Dougados et al. 246 patients with AS took celecoxib 200 mg, ketoprofen 200 mg or placebo for 6 weeks. There was no significant difference in the analgesic effect of both NSAIDs, although they were significantly superior to placebo. Of particular interest is the effect of NSAIDs on symptoms such as night pain and morning stiffness, which largely reflect an anti-inflammatory effect. The effects of ketoprofen and celecoxib were practically the same: the reduction in night pain averaged 21 and 27 mm VAS (in the placebo group it increased by 13 mm), morning stiffness decreased by 16 and 17 minutes (it did not change in the placebo group). Thus, ketoprofen has a clear anti-inflammatory effect in AS. Interestingly, the number of gastrointestinal complications while taking coxib and ketoprofen did not differ: they occurred in 13% and 14% of patients (8% on placebo) [21]. When discussing the safety of ketoprofen, one cannot ignore the fact that a number of population-based studies demonstrate a significant risk of gastrointestinal complications for this drug. Thus, J. Castellsague et al. conducted a meta-analysis of 28 epidemiological studies (1980–2011), which assessed the development of gastrointestinal complications when using various NSAIDs. The lowest risk was observed for celecoxib - OR 1.45, aceclofenac 1.4 and ibuprofen - 1.84. The danger was significantly higher when using diclofenac - 3.34, meloxicam - 3.47 and nimesulide - 3.83. Ketoprofen was among the top three drugs with the highest risk - 3.92, as well as naproxen - 4.1 and indomethacin - 4.14 [22].
On the other hand, one of the largest population studies showed a relatively low risk of gastrointestinal complications for ketoprofen. This work by Finnish scientists A. Helin-Salmivaara et al., based on an assessment of the causes of 9191 cases of gastrointestinal bleeding, ulcers and perforation, noted from 2000 to 2004. The control group consisted of 41,780 individuals matched by gender and age. The risk of gastrointestinal complications when using ketoprofen was lower compared to diclofenac: OR 3.7 and 4.2, respectively. Interestingly, ketoprofen showed a similar or even lower risk of developing gastrointestinal pathology than more selective NSAIDs (with the exception of celecoxib). Thus, the OR for meloxicam, nimesulide and etoricoxib was 3.4, 4.0 and 4.4, respectively [23].
It should be noted that Russia has accumulated extensive experience in the use of ketoprofen. In particular, a number of clinical studies were conducted in our country, the results of which showed not only the good therapeutic potential of this drug, but also a low incidence of complications [24, 25].
Among them, the work of L. B. Lazebnik et al. should be highlighted, in which a 3-month comparison of 4 NSAIDs: lornoxicam, nimesulide, celecoxib and ketoprofen was carried out in 132 patients with OA. The authors studied the risk of gastrointestinal complications and daily dynamics of blood pressure (BP). Ketoprofen demonstrated good tolerability: the number of patients with erosions and ulcers after using lornoxicam was 66% (!), nimesulide - 13.5%, ketoprofen - 13.0%, celecoxib - 8.3%. Increased blood pressure over 130/90 mm Hg. Art. was noted in only 2% of patients receiving ketoprofen. With regard to lornoxicam and nimesulide, the situation was completely different: in patients taking these drugs, an increase in blood pressure was noted in 11% and 13% [26] (Fig. 2). This work shows one of the most valuable advantages of ketoprofen - the relatively low risk of cardiovascular complications.
The association between ketoprofen use and CV accidents has been determined in several epidemiological studies. Thus, the low risk of MI when using ketoprofen was shown by American scientists G. Singh et al. Having analyzed the causes of 15,343 episodes of myocardial infarction (61,372 people constituted the corresponding control), the authors compared the frequency of this complication in people taking NSAIDs. It turned out that taking ketoprofen was associated with the lowest risk of MI (OR 0.88), even in comparison with naproxen (OR 1.08), which is traditionally considered the safest drug in relation to CV events [27].
Similar results were obtained by M. Solomon et al., who compared the use of various NSAIDs in 4425 patients who developed MI and 17,700 individuals without this complication. According to the data obtained, there was no difference in the intake of ketoprofen in these groups: 53 patients who developed MI (1.2%) and 190 control subjects (1.1%) received it. Thus, the use of ketoprofen, according to this study, did not increase the risk of developing HF accidents [28].
A low risk of CV complications for ketoprofen was also shown by the results of a population study by Finnish scientists A. Helin-Salmivaara et al. Their work was based on a comparison of data on NSAID use in 33,309 post-MI patients and 138,949 healthy people. It turned out that taking ketoprofen did not actually increase the risk of developing HF accidents (OR 1.11) [29].
In 2012, a large-scale study was published by scientists from Taiwan who studied the CV risk when using various NSAIDs in their own population. The study material was obtained using data from the national health system, which had information on 13.7 million people who used NSAIDs, of whom 8354 had a myocardial infarction. Oral ketoprofen showed minimal risk (OR 1.17). It was found to be safer than the vast majority of other NSAIDs (Figure 3).
It should be noted that parenteral use of NSAIDs (this was a separate section of the analysis) was associated with a higher risk of LE complications. Thus, for ketoprofen the risk was more than doubled: OR 2.34; a similar value was obtained for diclofenac: 1.88, and a significantly higher value for ketorolac: 4.27 [30].
Thus, ketoprofen is a universal analgesic that can be successfully used for both acute and long-term control of chronic pain. Favorable pharmacological properties determine its advantages in comparison with other NSAIDs for urgent pain relief, when the speed of relief of suffering is of fundamental importance. The presence of different dosage forms in the doctor’s arsenal helps when choosing an analgesic therapy strategy: to obtain the fastest possible effect in the first days of treatment, the use of parenteral forms of ketoprofen may be justified, followed by a transition to regular oral administration. A positive point is also the presence on the pharmacological market of high-quality and inexpensive generics of ketoprofen, such as Flamax® (Sotex), available to most patients.
Of course, ketoprofen is not without its drawbacks; the main one, typical of all “traditional” NSAIDs, is the possibility of developing gastrointestinal pathology. However, careful consideration of risk factors before prescribing NSAIDs and, if relevant factors are present, prophylactic use of gastroprotectors (proton pump inhibitors) can significantly reduce this danger. But at the same time, ketoprofen shows a low risk of complications from the cardiovascular system. This is an undoubted advantage that expands the possibility of using this drug in elderly people, many of whom have cardiovascular risk factors.
Literature
- Nasonov E. L. Analgesic therapy in rheumatology: a journey between Scylla and Charybdis // Klin. Pharmacol. therapy. 2003; 12 (1): 64–69.
- Pain (a practical guide for doctors). Ed. Yakhno N.N., Kukushkina M.L.M.: Publishing house of the Russian Academy of Medical Sciences, 2012. 512 p.
- Lee Y. Effect and treatment of chronic pain in inflammatory arthritis // Curr Rheumatol Rep. 2013; 15 (1): 300.
- Karateev A. E., Yakhno N. N., Lazebnik L. B. et al. The use of non-steroidal anti-inflammatory drugs. Clinical recommendations. M.: IMA-PRESS, 2009. 167 p.
- Varas-Lorenzo C., Riera-Guardia N., Calingaert B. et al. Myocardial infarction and individual nonsteroidal anti-inflammatory drugs meta-analysis of observational studies // Pharmacoepidemiology and Drug Safety. 2013; 22:559–570.
- Veys E. 20 years' experience with ketoprofen // Scand J Rheumatol Suppl. 1991; 90: Suppl 1–44.
- Sarzi-Puttini P., Atzeni F., Lanata L. et al. Pain and ketoprofen: what is its role in clinical practice? // Reumatismo. 2010, 62(3): 172–188.
- Venegoni M., Da Cas R., Menniti-Ippolito F., Traversa G. Effects of the European restrictive actions concerning nimesulide prescription: a simulation study on hepatopathies and gastrointestinal bleedings in Italy // Ann Ist Super Sanita. 2010; 46 (2): 153–157.
- Kokki H. Ketoprofen pharmacokinetics, efficacy, and tolerability in pediatric patients // Paediatr Drugs. 2010; 12 (5): 313–329.
- Díaz-Reval M., Ventura-Martínez R., Déciga-Campos M. et al. Evidence for a central mechanism of action of S-(+)-ketoprofen // Eur J Pharmacol. 2004; 483(2–3):241–248.
- Barden J., Derry S., McQuay H., Moore R. Single dose oral ketoprofen and dexketoprofen for acute postoperative pain in adults // Cochrane Database Syst Rev. 2009, Oct 7; (4): CD007355.
- Glina S., Damiao R., Afif-Abdo J. et al. Efficacy and safety of parecoxib in the treatment of acute renal colic: a randomized clinical trial // Int Braz J Urol. 2011; 37(6):697–705.
- Karvonen S., Salomäki T., Olkkola K. Efficacy of oral paracetamol and ketoprofen for pain management after major orthopedic surgery // Methods Find Exp Clin Pharmacol. 2008, 30(9): 703–706.
- J. Olson N., Otero A., Marrero I. et al. Onset of analgesia for liquigel ibuprofen 400 mg, acetaminophen 1000 mg, ketoprofen 25 mg, and placebo in the treatment of postoperative dental pain // Clin Pharmacol. 2001, 41(11): 1238–1247.
- Jokhio I., Siddiqui K., Waraich T. et al. Study of efficacy and tolerance of ketoprofen and diclofenac sodium in the treatment of acute rheumatic and traumatic conditions // J Pak Med Assoc. 1998; 48: 373–376.
- Sarzi-Puttini P., Atzeni F., Lanata L., Bagnasco M. Efficacy of ketoprofen vs. ibuprofen and diclofenac: a systematic review of the literature and meta-analysis // Clin Exp Rheumatol. 2013 Sep-Oct; 31 (5): 731–8. Epub 2013 May 17.
- Dib M., Massiou H., Weber M. et al. Efficacy of oral ketoprofen in acute migraine: a double-blind randomized clinical trial // Neurology. 2002, 58(11): 1660–1665.
- Altman R., Honig S., Levin J., Lightfoot R. Ketoprofen versus indomethacin in patients with acute gouty arthritis: a multicenter, double blind comparative study. J Rheumatol. 1988, 15(9): 1422–1426.
- Le Loet X. Safety of ketoprofen in the elderly: a prospective study on 20,000 patients // Scand J Rheumatol Suppl. 1989; 83:21–27.
- Schattenkirchner M. Long-term safety of ketoprofen in an elderly population of arthritic patients // Scand J Rheumatol Suppl. 1991; 91:27–36.
- Dougados M., Béhier J., Jolchine I. et al. Efficacy of celecoxib, a cyclooxygenase 2-specific inhibitor, in the treatment of ankylosing spondylitis: a six-week controlled study with comparison against placebo and against a conventional nonsteroidal antiinflammatory drug // Arthritis Rheum. 2001, 44(1):180–185.
- Castellsague J., Riera-Guardia N., Calingaert B. et al. Individual NSAIDs and upper gastrointestinal complications: a systematic review and meta-analysis of observational studies (the SOS project) // Drug Saf. 2012; 35(12):1127–1146.
- Helin-Salmivaara A., Saarelainen S., Gronroos J. et al. Risk of upper gastrointestinal events with the use of various NSAIDs: A case-control study in a general population // Scan J Gastroenterol. 2007; 42:923–932.
- Chichasova N.V., Immametdinova G.R., Karateev A.E. et al. Efficacy and safety of ketoprofen (ketonal) for rheumatoid arthritis (clinical and endoscopic study) // Scientific and practical rheumatology. 2001; 1; 47–52.
- Osipova N. A., Petrova V. V., Ermolaev P. M., Beresnev V. A. Nonsteroidal anti-inflammatory drugs in the treatment of postoperative pain in cancer patients // Pharmateka. 2006, no. 6, 121.
- Lazebnik L. B., Drozdov V. N., Kolomiets E. V. Comparative effectiveness and safety of ketoprofen, lornoxicam, nimesulide and celecoxib in patients with osteoarthritis // RMJ. 2004, 12 (14), 844–847.
- Singh G., Mithal A., Triadafilopoulos G. Both selective COX-2 inhibitors and non-selective NSAIDs increase the risk of acute myocardial infarction in patients with arthritis; selectivity is with patients, not the drug // Ann Rheum Dis. 2005, 64 (suppl 3), 85.
- Solomon D., Glynn R., Levin R., Avorn J. Nonsteroidal Anti-inflammatory Drug Use and Acute Myocardial Infarction. Arch Intern Med. 2002; 162:1099–1104
- Helin-Salmivaara A., Virtanen A., Vesalainen R. et al. NSAID use and the risk of hospatalization for first myocardial infarction in the general population: a national case-control study from Finland // Eur Heart J. 2006; 27:1657–1663.
- Shau W., Chen H., Chen S. et al. Risk of new acute myocardial infarction hospitalization associated with the use of oral and parenteral non-steroidal anti-inflammation drugs (NSAIDs): a case-crossover study of Taiwan's National Health Insurance claims database and review of current evidence // BMC Cardiovasc Disord. 2012, Feb 2; 12: 4. doi: 10.1186/1471–2261–12–4.
A. E. Karateev, Doctor of Medical Sciences, Professor
FSBI NIIR named after. V. A. Nasonova RAMS, Moscow
Contact Information
Patient reviews
Yulia, 27 years old, Nizhny Novgorod: “I met Ketorol just a year ago. A friend advised me to take a pill when I had a toothache. Since then I have kept this medicine in my home medicine cabinet. I try not to overuse it. And recently I had such a headache that I had to take the pill again. Helped almost immediately. I recommend".
Leonid, 61 years old, Krasnoyarsk: “My daughter brought Ketanov about six months ago, when he complained to her of severe pain in his knees. The drug helps well, but my daughter warned me not to use it too often. I only take pills when the pain is unbearable.”
Clinical picture
The key symptom of the disease is pain, but its nature can vary, as can the accompanying clinical signs:
- with pulpitis, the pain subsides during the day and increases in the evening, having a wave-like character and intensifying with physical contact of the tooth with any object;
- with periodontitis, the pain is more intense and does not subside for a minute, which is associated with damage to the bone tissue around the apexes of the roots. Damage to the ligamentous apparatus and the breakdown of nerve tissue not only causes discomfort, but also makes the tooth itself mobile, and any movement of it in the socket is accompanied by a new attack of pain;
- if the cause of the disease is an abscess, then the periodontium around it will differ from healthy tissue by the presence of edema and hyperemia, complemented by a feeling of pulsation in the gums. A localized abscess in some situations does not cause pain if the nerve endings have died, but this scenario can lead to the development of osteomyelitis.
Reviews from doctors about Ketorol and Ketanov
Igor, 40 years old, neurologist, Samara: “Ketorol is an effective pain reliever that can quickly eliminate pain in inflammatory joint pathologies. But I prescribe it for a short period of time, only at the beginning of the development of the disease, in order to alleviate the patient’s condition.
The drug has many contraindications that should be taken into account. But the medicine has a great advantage - several forms of release make it possible to take the medicine internally, give injections and apply externally.”
We recommend reading: Chondroxide - treatment and prevention of osteoarthritis and osteochondrosis of the spine
Olga, 48 years old, dentist, Khabarovsk: “For severe pain that occurs after the removal of a wisdom tooth, I prescribe Ketanov. The tablets quickly relieve pain. I warn patients that they should not take this medicine often or for a long time, as unpleasant consequences are possible. The medication has many contraindications and side effects are possible.”
Which drug is better?
Even a specialist will not give an exact answer to this question. When determining the appropriate remedy, the doctor takes into account many factors. You should not take these medications without first consulting a doctor.
Joint diseases
"Ketorol" effectively eliminates joint pain, and "Ketanov" blocks the development of inflammation that occurs in the tissues of the joints.
Toothache
In this case, “Ketanov” is more suitable. It is often prescribed after the removal of a wisdom tooth, because its roots are located deep in the jaw and after the operation the patient feels acute, severe pain. Wounds take a very long time to heal, so it is necessary to take painkillers. The dosage can only be prescribed by the attending physician. The appointment is carried out according to the exact instructions of the dentist.
How to replace Linux with a cheaper one
Oncological diseases
For severe pain in oncology, only Ketorol is prescribed. Other medications in this case will be powerless.
Osteochondrosis
Thanks to the anti-inflammatory effect, Ketorol quickly relieves inflammation and blocks pain. This drug is ideal for patients with osteochondrosis. However, before taking it you need to familiarize yourself with the contraindications. If for some reason the drug is not suitable, then it is better to stop taking it and choose an equally effective medicine.