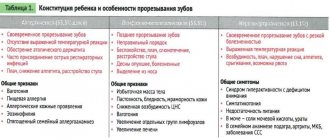
Scarring
Healing of a granulating wound occurs through scarring and epithelization. At the final stage of healing, collagen fibers appear among the cells of the granulating tissue, the number of granules decreases, and the number of fibers increases. Ultimately, the fibrous substance passes into the connective tissue and forms a scar.
When wounds heal by primary intention, delicate scar tissue is formed, which tends to resolve.
In case of healing by secondary intention, a rough scar is formed, which will not be easy to get rid of.
Types of wound healing
According to the classification of I.V. Davydkovsky, the following types of wound healing are distinguished:
- closing the defect of the epithelial cover, which occurs when the upper epithelial layer is damaged;
- healing under a scab, or healing without a scar. Observed on mucous membranes in case of minor defects.
- healing by primary intention, or healing without suppuration. Characteristic of wounds with damage to the skin and tissue underneath.
- healing by secondary intention, or healing through suppuration and granulation. Occurs with extensive wounds, accompanied by foreign objects entering the wound, tissue necrosis, microbes and infections.
Indications for secondary intention
When there is a high risk of infection, surgeons choose secondary intention of damaged soft tissue. Necessary conditions for treatment:
- Abundant microbial insemination of the injured surface.
- Large wound size.
- The presence of foreign bodies, dirt, necrotic tissue, and blood clots in the pathological cavity.
- Diseases for which the patient is not indicated for serious surgical interventions followed by excision of a large amount of tissue. Secondary intention is a safer method.
Important factors for determining the tactics of surgical treatment are the contamination of the injury with pathogenic microorganisms and the distance between the edges of the wound. The healing process can be accelerated by excision of the affected flaps. To improve the effect of the operation, drug therapy is prescribed.
Stages of healing
The wound healing process goes through three main stages: inflammation, regeneration, and restoration of the epithelium.
The inflammation phase begins immediately after injury and in an uncomplicated state lasts for 4–5 days. During the hemostasis stage, platelets attach to sites of injury and cause a chemical reaction that activates fibrin, which forms a matrix network and binds platelets to each other. This is how blood clots form, blocking damaged blood vessels and stopping bleeding.
At the stage of proliferation and regeneration, the process of angiogenesis, collagen deposition, and the formation of granulation tissue (young connective tissue formed in places of defects) occurs. The regeneration stage can last 2–4 weeks depending on the size of the defect.
The final stage is the formation of the epithelium. Depending on the severity of the injury, the process can last from several weeks to a year or more.
Every year in Russia more than 25 thousand cases of rectal and anal cancer are detected [1]. With all the advances in the field of radiation therapy, surgery remains the main treatment method for this category of patients. Back in 1908, E. Miles [36] proposed an original technique for removing the rectum along with its obturator apparatus, which for a long time remained the “gold standard” for the treatment of rectal cancer. The number of abdominoperineal extirpations (APEs) performed has decreased from 90% in the 70s to 37% by the end of the 20th century [34].
After BPE, a volumetric defect is formed in the perineal tissues. Despite various options for its plastic closure, complications of the perineal wound are observed on average in 38% of patients [64]. There is no consensus on the optimal management of this category of patients.
Healing of a perineal wound is influenced by a number of factors: the volume of the defect, the amount of exudate, bacterial contamination, previous chemoradiotherapy (CRT), the granulation process, etc. [4].
Modern management of complicated perineal wounds involves the use of various absorbent dressings, depending on the phase of the wound process: alginate, hydrofiber, sponge, interactive super-absorbent, but this method is associated with a long hospital stay, the need for frequent, painful dressings and the significant cost of consumables [22]. Vacuum therapy (VAC) is a promising method for treating long-term non-healing wounds, but the experience of its use in perineal wounds is limited to isolated cases [15, 47].
An uninfected perineal wound after BPE of the rectum in the absence of tension can be sutured layer-by-layer without plastic manipulation [45]. The main advantage of direct suturing of the perineal wound is the minimum additional operation time (Fig. 1, a).
Rice. 1. Options for plastic closure of a perineal wound. a — direct suturing of the defect; b — plastic surgery of the defect with local tissues; c — VY-skin plasty; d — plastic surgery of the perineal defect using the rectus abdominis muscle. Arrows indicate the directions of traction of tissues or flaps.
For extensive wounds of the perineum, plastic surgery of the defect with local tissue is used - a method of closing the wound through rotation or transposition of the aponeurotic skin flap [52], with the main source of blood supply being the internal pudendal artery [55]. The most illustrative examples of the use of regional flaps are Lotus and Singapore. The Singapore flap was described by J. Wee and V. Joseph in 1989 [63]. With this method, a flap of tissue lateral to the labia majora is cut out posteriorly and transposed medially. The lotus flap [65] is a skin-aponeurotic flap, shaped like a petal of a lotus flower, and in case of multiple plastic surgery, the flower itself (see Fig. 1, b).
Pedicled flaps are transplanted from another anatomical area while preserving the vascular pedicle. The main donor areas are the abdomen, inner thigh and buttocks. The use of musculocutaneous flaps (plasty with the rectus abdominis or gracilis muscle) is advisable when filling volumetric defects. Gracilis muscle grafting was described by McCraw in 1976 [6]. The main disadvantage of the method is the segmental blood supply to the gracilis muscle, which requires bilateral mobilization of the flap. Modified by J. Soper et al. [57] involves a shorter gracilis muscle flap, with the pedicle taken more medially, which provides higher flap mobility and the need for only 90° rotation. In plastic surgery of the gluteal muscles, a full-thickness flap is isolated, fed from the inferior gluteal artery. This technique is very reliable and technically quite easily reproducible; it is mainly used to close posterior perineal defects, but can also be used in other situations [2, 25]. VY-skin plasty is one of the possible methods for plasty of the perineal defect; The blood supply to the flaps comes from the gluteal arteries. This type of plastic surgery includes the mobilization of two full-thickness triangular flaps on either side of the defect and Y-type suturing [8] (see Fig. 1, c).
Plastic surgery of the perineal defect using the rectus abdominis muscle was described by H. Shukla and L. Hughes in 1984 (see Fig. 1, d) [54]. The flap is supplied with blood from the deep inferior epigastric vessels, which penetrate the muscle and supply the skin of the abdomen. During mobilization, the caudal end of the flap is crossed, and the flap is brought down through the defect in the pelvis to the perineum [59, 60]. The main disadvantage of the method is the frequent formation of a hernia of the anterior abdominal wall.
Omentoplasty involves bringing down a portion of the omentum on the stem into the pelvic cavity. It is believed that omentoplasty in combination with primary closure prevents the accumulation of fluid in the “dead” space of the small pelvis and prevents fusion of the small intestine with the pelvic floor, thereby reducing the incidence of wound infection, hernia and small bowel obstruction [27], and when combined with VAC therapy reduces the likelihood of perineal small intestinal fistulas [15].
Plastic surgery of a perineal defect with a biograft is a technique that involves plastic surgery of a pelvic defect with noncellular material obtained from the dermis of pigs, the submucosal layer of the intestine, and the intercellular space of the human dermis [18]. The biological graft facilitates revascularization; it has a honeycomb structure, which ensures its ingrowth and remodeling in the recipient's body. According to O. Peacock et al. [49], the use of biotransplants reduces the duration of the operation and eliminates the need for the participation of a plastic surgeon; in addition, it is assumed that the use of biograft has a low rate of complications and rejection, as well as higher cost-effectiveness. However, convincing data on the results of using this method are currently lacking. Only a few cases of plastic surgery of a perineal defect with a synthetic allograft have been described [16]. The perineal wound after BPE is characterized by bacterial contamination, which increases the risk of infectious complications and rejection of the synthetic mesh [55]. Most of the methods listed above are difficult to reproduce and require the participation of plastic surgeons in the operation.
Regardless of the method of closure, wound healing is a complex process of sequential immunological and biological interactions that includes a cascade of events accompanied by the appearance of different cell types at different phases of the wound process [11, 28]. The healing process can be described as a sequence of several stages: 1) coagulation; 2) inflammation; 3) proliferation; 4) granulation and epithelization [11, 28]. Parts of the wound can simultaneously be in different stages of healing [9, 51]. The end result is a mature scar with few vessels and high strength [24, 44]. When the edges of the wound touch, in the absence of foreign bodies in the wound and infection, the wounds heal by primary intention [23]. If there is a large tissue defect, wounds heal by secondary intention. Compared to wound healing by primary intention, this process takes longer and requires more granulation tissue [50]. Wound healing is influenced by many local (edema, ischemia, tissue hypoxia, infection, necrosis and imbalance of growth factors) and systemic (metabolic diseases, perfusion disorders or concomitant diseases) factors [4].
Preoperative CRT, which is often prescribed to patients with rectal and anal cancer, has a particular impact on the repair processes. This type of treatment provides benefits in terms of local disease control, reduces the risk of recurrence, and improves survival rates, but also significantly increases the risk of wound complications. In a retrospective review, K. Bullard et al. [12] analyzed the results of treatment of 160 patients with rectal cancer who underwent BPE with primary closure of the perineal wound. In this study, the perineal wound complication rate was 41%; with neoadjuvant CRT, this figure increased 2-fold - from 23 to 47%. Similar results were obtained by D. Artioukh et al. [4]. In the CRT group, the number of non-healing perineal wounds was 39.1% compared to 6.7% in the non-healing group. Salvage therapy for squamous cell carcinoma of the perianal skin and anal canal is also associated with a high rate of perineal wound complications after CRT (47-80%) [43, 48, 62]. The side effect of CRT on perineal wound healing is directly related to damage to normal tissues due to occlusive vasculitis and fibrosis [58]. In the pelvis, radiation fibrosis limits the ability to close the perineum and lateral pelvic wall, increasing the risk of complications.
Other factors related to comorbidities also increase the risk of perineal wound complications. Diabetes mellitus, low preoperative hematocrit, tumor size, and obesity are significant predictors of perineal wound complications [14].
Complications of a perineal wound can be observed even with careful surgical technique, adequate hemostasis and drainage of the “dead” space of the small pelvis. Minor complications of a perineal wound include cutting of skin sutures, excessive granulation, and the formation of a residual cavity in the pelvis. More serious complications include abscess of the pelvic cavity and diastasis of the perineal wound. If there is an abscess or cavity in the pelvis and the wound cannot heal by secondary intention, opening the wound is usually sufficient to ensure adequate drainage. In the case of diastasis of the perineal wound and in the absence of loops of the small intestine in the wound cavity, the management of the perineal wound is carried out using absorbent bandages.
It has been proven that wounds heal better in a moist, warm and clean environment [46]. Currently, it is common to use several types of modern dressings that provide a moist environment for favorable wound healing.
During the exudative phase of wound healing, superabsorbent dressings of the sorption-washing type are effective, maintaining a moist environment, ensuring sanitation of the wound and helping to clean the wound from necrotic masses. Dressings of this type can remain on the wound for up to 3 days and are easily separated from the wound surface due to their low tendency to stick [19].
Alginate dressings are widely used after surgery to fill defects in open wounds. When this type of dressing comes into contact with a wound, calcium ions in the dressing are exchanged for sodium ions in the serum or wound discharge. When a significant portion of the ions is replaced, the fiber absorbs exudate, swells and partially dissolves to form gel-like masses, which ensures painless removal of the dressing [17]. For infected wounds, silver-containing alginate dressings with an antiseptic effect are applicable [56].
Hydrofiber dressings contain carboxymethylcellulose fibers, which, when in contact with the wound surface, form a gel that provides a favorable environment for healing, unidirectional outflow of exudate and adequate ion exchange. The fibrin formed in this case ensures adequate adhesion of the dressing without tissue ingrowth into it. This type of dressing often contains silver ions and is used for the management of contaminated wounds [29].
Foams, silicone elastomers, polyurethane foam sponges or other hydropolymer dressings have pronounced absorbent properties and can absorb liquids up to 10 times their own dry mass [5]. This type of dressing is more effective than hydrocolloid dressings but is equivalent to alginate dressings for the management of severely exuding wounds. This type of dressing does not shorten wound healing time, but reduces discomfort, is cheaper and is associated with an earlier transfer of the patient to outpatient follow-up care [40].
Hydrocolloid dressings consist of two layers. The inner, hydrocolloid layer has particles that absorb exudate and form a hydrated gel, which creates a moist environment. The outer layer—film, foam, or a combination of both—forms a dense cover that protects against bacterial contamination of the wound, ingress of foreign particles and secretions [41]. Hydrocolloid dressings are most often used for chronic wounds that require frequent changes. They can be used at different stages of the wound process, including necrotic wounds, eschar, granulating and infected wounds [42].
Several therapeutic methods are also used to manage complicated perineal wounds: hydrotherapy, enzymatic debridement, the use of growth factors and VAC therapy [53].
Hydrotherapy (using lavage or the collection method) helps to cleanse the wound, but with long-term use it is inappropriate due to the delay in the formation of granulation tissue caused by it, and therefore is not used in routine practice [53]. Treatment of the wound with enzymes and the use of growth factors accelerate the repair process, however, there have been no large randomized studies on this issue [26, 35].
Vacuum dressings entered medical practice in 1995 and were designed to reduce the time of wound healing by secondary intention [13]. The vacuum dressing consists of a negative pressure system, a polyurethane sponge and a drainage system. A non-kink, penetrated drainage system is connected to a sponge and is brought out parallel to the skin. The polyurethane sponge is cut to fit the size of the wound and sealed with a film to create a closed system. Negative pressure is set within the range of 20-125 mmHg. The vacuum dressing is usually changed every 48-72 hours depending on need [31]. Pain when changing the dressing is usually moderate and stops 30 minutes after changing the dressing. The portability of the negative pressure device makes it possible to manage patients with a chronic wound without limiting their mobility [7, 10].
The mechanisms by which VAC therapy improves wound healing are being actively studied. Negative pressure therapy stimulates angiogenesis [13] and collagen release [37], which is one of the most important conditions for the formation of granulation tissue. Discharge from chronic wounds contains a large amount of pro-inflammatory agents, matrix metalloproteinases and protease inhibitors, which have a negative effect on the healing process. VAC therapy promotes effective evacuation of excess exudate from the wound and accordingly reduces the concentration of inflammatory mediators. Among other benefits, VAC therapy reduces bacterial contamination of the wound, increases the oxygen concentration in the wound and mechanically brings the edges of the wound closer together [30, 39]. Clinical trials have shown that VAC therapy increases granulation tissue formation and reduces wound volume [3, 20]. The literature describes isolated cases of VAC therapy for wounds after BPE [15, 47]. In 2008, S. Cresti et al. [15] published a successful clinical experience of using VAC therapy in 2 patients suffering from cancer of the lower ampullary rectum due to Crohn’s disease and cancer of the anal canal, after BPE with plastic surgery of the perineal defect with a greater omentum. In one case, the operation was preceded by CRT SOD 60 Gy. The wound surface during negative pressure therapy in the described patients decreased from 10x10 and 20x17 cm2 after surgery to 4x6 and 12x9 cm2 by the 12th day of therapy. Unfortunately, despite the fact that the authors were guided in prescribing VAC therapy by infection of the perineal wound, data from bacteriological studies are not provided. The patients were discharged from the hospital on the 13th and 25th days after the interventions.
Negative pressure therapy comes with certain risks and complications. The most common complication is wound suppuration; in most cases it is associated with untimely change of the vacuum dressing. Bleeding is a serious complication that can occur due to wound infection and when the dressing is removed. Patients receiving anticoagulant therapy are also at risk. Sometimes hospitalization, surgery, and blood transfusions are required to stop bleeding [61].
According to the Pennsylvania Patient Safety Reporting System (PA-PSRS), nearly half of negative pressure therapy complications are associated with inadequate wound care and monitoring after vacuum dressing placement [33]. Education of both medical personnel and patients and their caregivers is an important component of the successful use of local negative pressure. The educational program for patients and caregivers should include the following points: safe operation of the device (providing printed instructions to patients and caregivers), troubleshooting against the background of audio and video warning signals, removing the old dressing and installing a new one, recognizing the first symptoms of complications and an action plan when they appear (for example, the appearance of scarlet blood in a suction tube or container requires immediate assistance from medical personnel) [21, 32, 38].
We present our own clinical observation in which VAC therapy was used for a complicated perineal wound after BPE.
Sick
, 61 years old, with a 3-year history of condylomas in the perianal area, applied to the State Research Center named after. A.N. Red due to the rapid growth of condylomas over the past 6 months. MRI data: in the perianal area with transition to the right and left gluteal areas, a space-occupying formation of up to 30 cm in the greatest dimension is determined. A tumor of heterogeneous structure with foci of decay. Its upper pole extends to all portions of the external sphincter, the intersphincteric space, and is adjacent to the distal parts of the levator. The middle and lower third of the anal canal cannot be traced; one of the tumor components extends to the root of the scrotum. No other manifestations of the disease were found.
Due to suspected malignancy of the tumor, almost complete destruction of the anal sphincters, as well as complete anal incontinence, on January 30, 2015, a BPE of the rectum was performed with wide excision of the skin of the perineum, with the formation of an intra-abdominal colostomy; Taking into account the extensive perineal defect, VY-skin plasty was performed (Fig. 2). The pelvic cavity is drained from the perineum through a separate counter-aperture. Due to wound contamination, as well as for additional drainage of exudate, silver-containing hydrofiber dressings were installed intraoperatively. Histological conclusion: squamous cell carcinoma, in some areas with a tendency to keratinization, growing into the adjacent tissue, external and internal sphincters.
Rice. 2. Perineal stage of extralevator abdominal-perineal extirpation of the rectum with the formation of an intra-abdominal colostomy, VY-skin plasty. a — Buschke-Levenshtein tumor; b — view of the perineal wound during removal of the drug; c — V-type mobilization of the flap; d — view of the perineum after VY-skin plasty.
From the 1st to the 9th day, the sutures on the perineal wound were intact. The pain syndrome was moderate; dressings required additional intramuscular injection of non-narcotic analgesics. During this period, dressings were carried out using absorbent and alginate dressings. Subjectively, the patient noted discomfort in the area of the perineal wound, which limited his mobility. The amount of exudate from the 1st to the 8th day after surgery averaged 200 ml per day; by the 9th day, the discharge acquired a serous-purulent character. Bacteriological study of culture from the bottom of the wound: the dominant flora is Enterobacter cloacae
109 CFU, resistant to all antibacterial drugs available in the clinic. On the 10th day, cutting of the sutures of the perineal wound in the central part with diastasis of the wound edges of up to 10 cm was detected; the patient noted an increase in temperature in the evening to 38.3 °C. During revision, the volume of the wound was 700 cm3. Fibrin deposits along the edges and bottom of the wound. Granulations are sluggish. In the area of the coccyx there is a zone of tissue necrosis up to 5 cm in greatest dimension (Fig. 3, a). Under local anesthesia, the wound was sanitation and necrectomy was performed. In order to optimize wound management, it was decided to use the local negative pressure method.
Rice.
3. Condition of the wound on the 10th and 19th days after surgery. a — condition of the wound before the start of VAC therapy (10th day after BPE); b, c, d — dressing on the 19th day after BPE (8th day of VAC therapy); b - general view; c — to prevent the formation of fistulas, a collagen and sponge dressing is placed at the bottom of the wound; d — VIVANO system is installed. Under anesthesia (NSAID), the VIVANO system was installed in a constant aspiration mode of 100 mm Hg. Due to the anatomical features of this area and the presence of natural folds, the surface is leveled using insulating hydrocolloid plates and sealant paste. To prevent the formation of fistulas, a collagen and sponge dressing is placed at the bottom of the wound. The vacuum dressing was changed every 3 days, which significantly saved the labor costs of medical personnel.
On the 8th day, when assessing the results of VAC therapy, a reduction in the size of the wound to 500 cm3 is noted (see Fig. 3, b), a decrease in the amount of exudate to 160 ml. When the bandage is removed, severe tissue bleeding is observed, the edges of the wound are viable. There is no fibrin plaque. Material for sowing was taken from the bottom of the wound. Bacteriological research data: the dominant flora is Staphyloccus xylosus
109 COE.
On the 15th day of VAC therapy, the wound was clean, with a volume of 200 cm3. Pronounced granulations are noted (Fig. 4, a). Culture revealed Escherichia
coli
108 CFU. Under local anesthesia, functional provisional sutures were applied to gradually close the perineal defect (see Fig. 4, b).
Rice.
4. Condition of the wound on the 26th day after surgery (a, b), at discharge on the 34th day (c) and after radiation therapy (d). The amount of exudate was 300 cm3 per day during the first 4 days and decreased to 30 cm3 in the last 3 days of VAC therapy. Subjectively, the patient noted an improvement in his general condition from the first day of VAC therapy, less discomfort during physical activity, and less need for painkillers.
The patient was discharged from the hospital on the 34th day after surgery. Further dressings using alginate and ointment dressings were carried out on an outpatient basis.
After the final healing of the perineal wound, the patient received a course of adjuvant radiation therapy with a dose of 50 Gy. The condition of the perineal wound at discharge and after radiation therapy is shown in Fig. 4, c and 4, d, respectively.
In summary, local negative pressure dressings for complicated perineal wounds are a feasible and reproducible technique. Potentially, this technique makes it possible to reduce the healing time of perineal wounds; it also has advantages in the form of stimulation of the granulation process, reducing the volume of the wound, increasing blood flow in the wound in the area of negative pressure and reducing bacterial contamination of the wound, which is well tolerated by the patient.
The use of vacuum therapy in the treatment of perineal wounds is associated with certain limitations, since due to the anatomical features and the presence of multiple folds in this area, corresponding difficulties may arise in ensuring the tightness of the system. In addition, the use of the local negative pressure method is associated with certain risks and contraindications. In this regard, it is necessary to carefully select patients according to individual indications. There have been no studies of the effectiveness of vacuum therapy in the treatment of wounds after abdominoperineal extirpation. The definitive role of vacuum therapy in the treatment of patients with complicated perineal wounds remains to be established.
Wound treatment
The choice of wound treatment method largely depends on their type (infected or necrotic, wet exuding or fibrous granulating, trophic ulcers or bedsores). Only a doctor can choose the optimal solution for treating each type of wound.
In addition, at each stage of wound healing, it is necessary to use a different agent: one that promotes the removal of exudate, the formation of granulation tissue, accelerating epithelization, etc.
When treating wounds, you need to remember that the wound does not heal on its own, but thanks to the body’s resources aimed at healing it. The immune, endocrine, and circulatory systems are involved in this process. A qualified doctor, along with treating the wound itself, will definitely prescribe a vitamin complex to maintain the body.
Clinical researches
Conducted clinical studies prove the high efficiency, safety and tolerability of the products. In VERTEX laboratories it was proven that La-Cri cream for sensitive skin reduces itching and irritation, relieves skin redness and moisturizes, gently cares for the skin.
Sources:
- Molochkova Yulia Vladimirovna, Dermatology. Brief reference book, GEOTAR-Media, 2022.
- Baumann Leslie, Cosmetic Dermatology. Principles and practice, MEDpress-inform, 2016.
- Ratner Desiri, Avram M.R., Avram M.M., Procedures in Dermatology. Clinical cosmetology, GEOTAR-Media, 2022.
How to speed up healing
The speed of wound healing varies. It depends on the nature of the injury and the individual characteristics of the patient, such as age, nutrition, and medications taken.
To speed up healing, it is necessary to provide optimal conditions for tissue regeneration at each stage. This role is fulfilled by therapeutic dressings designed for each stage of healing.
The method of hydrotherapy has a positive effect. Its essence consists in the sequential use of two dressings HydroClean and HydroTac. Using the first, the wound is cleaned, and then a second is applied, creating optimal conditions for granulation and epithelization.
What to do if the wound does not heal
Non-healing or chronic are wounds that do not respond adequately to therapy despite prolonged treatment. Such wounds are usually caused not by external factors, but by reasons hidden inside the body, leading to disruption of metabolic processes and, as a consequence, disruption of the wound healing process. This category includes trophic ulcers, bedsores, and diabetic foot ulcers. Before using any dressings, consult a doctor: therapy and treatment of wounds can only be prescribed to you by a doctor!
For the treatment of chronic wounds, HARTMANN has developed a two-bandage system - HydroClean Plus and HydroTac.
The HydroClean Plus cleansing dressing can be used at all stages of wound healing, effectively removing necrotic tissue and pathogenic bacteria from the wound surface. They get caught in the absorbent layer and die under the influence of the antiseptic. The HydroTac dressing has absorbent and moisturizing properties and also protects the wound from secondary infection.
With the help of the hydrotherapy system, many patients have been able to significantly alleviate suffering and improve their quality of life.