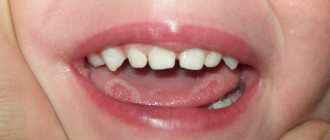
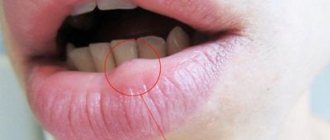
Causes of the problem
A red spot on the tongue can be a manifestation of a variety of pathologies, for example:
- Vitamin deficiency
Redness of the tongue is caused by a deficiency of B vitamins and niacin.
- Allergy
Response to food, drinks, drugs
- The burn is
not only thermal, but also chemical. The Internet is full of different, sometimes strange, advice. Experimenting on yourself can have sad consequences.
- Hormonal imbalance
Red spots on the tongue often appear in women during pregnancy and menopause.
- Infections of various etiologies
Bacteria and viruses provoke inflammatory processes, one of the symptoms of which is discoloration.
Red spots on the tongue are not yet a diagnosis. A doctor needs to conduct an examination to determine the exact cause.
Redness of the tongue may indicate various diseases.
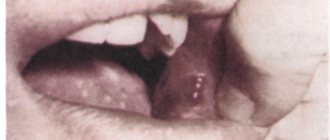
Red bumps on the tongue closer to the throat - what are they?
In most cases, bumps at the base of the tongue, pimples on the side, growths on the tip of the tongue are manifestations of the following diseases:
- Diseases of the mucous membrane of an inflammatory nature (glossitis) are accompanied by the formation of painful red rashes on the mucous membrane, in severe form - abscesses, phlegmons.
- Metabolic disorders, vitamin deficiency. Such conditions are characterized by redness and enlargement of the taste buds, which often become inflamed and acquire a red-white color.
- Herpes, characterized by the appearance of painful red pimples and blisters.
If red bumps or nodules appear on the base of the tongue, this may be a symptom of pyogenic granuloma. The formations consist of blood vessels and are localized in the wounded area. Pathology occurs due to injuries and damage to the mucous membrane. When touching the formations, a person feels a sharp pain.
- Digestive disorders (malabsorption). Pimples on the root, all over the surface of the tongue, are one of the symptoms of this pathology.
- Candidiasis (thrush). A disease that often affects newborns. The child's tongue becomes covered with red bumps and a cheesy coating forms. The baby behaves restlessly, cries, and has difficulty swallowing; these symptoms are caused by itchy red-white pimples and dry mouth.
- HPV – human papillomavirus. Formations are localized in any area of the tongue: at the tip, root, side. The bumps on the tongue closer to the larynx cause particular discomfort, as they interfere with swallowing and create the sensation of a foreign object in the mouth.
- Allergic diseases. The rashes do not hurt, but they interfere with swallowing and speaking.
- Diseases common to children: chickenpox, measles.
Diagnosis
It is difficult to independently distinguish relatively harmless manifestations of diseases in the form of red spots from serious disorders. Any rash on the tongue already indicates systemic problems, but some of them indicate serious cases.
Erythroplakia requires immediate surgical intervention. Therefore, it is better not to take the position “it will go away on its own,” but to consult a doctor.
Since spots on the tongue are a symptom of disease, examination is usually aimed at identifying the causes. Laboratory tests, flora tests, histology and medical history allow us to make the correct diagnosis and prescribe appropriate treatment.
What does a healthy tongue look like?
First, let's remind parents what a healthy tongue looks like. The following signs indicate the state of normality:
- the size is not increased;
- humidity is moderate;
- the color of the tongue is pale pink, without spots or grooves;
- sensitivity is normal, papillae are not enlarged;
- allow for a light coating that is easy to clean;
- There is no bad breath.
If, upon examination of the child, the condition of his tongue corresponds to the signs described above, there is no reason to worry and see a doctor.
Online consultation with a doctor if you are concerned about symptoms
If you are concerned about symptoms such as spots on the tongue, accompanied by burning, tingling, pain, then it is best to undergo an examination and consultation with a dentist. Because these may be signs of a more serious disease that should not be neglected, otherwise inaction will lead to the need for longer-term and more expensive treatment. Red spots on the surface of the tongue may indicate a fungal, viral, or venereal infection. It is often difficult to determine on your own what it is: glossitis, stomatitis, Kawasaki disease or something else. A specialist will help you understand the signs of the disease and etiology online. He will give professional recommendations, suggest treatment options and further actions.
Pathological plaque on the tongue
If the white coating on the tongue is caused by an illness, it persists throughout the day. A thin white coating occurs with any ARVI. It disappears as soon as the patient recovers.
Particular attention should be paid to the compaction of plaque. The body of the tongue is not visible through the thick coating. Such plaque is difficult to remove. Thick plaque is considered a sign indicating the severity of the disease.
The color of the coating on the tongue is also important. The more intense the color, the more serious the pathology that caused the plaque. The color of plaque is not only white. A yellowish tint to the plaque may be associated with a malfunction of the gallbladder or pancreas. Gray plaque is possible in case of stomach disease - gastritis, peptic ulcer. In some severe infectious diseases, plaque may acquire a black, bluish or greenish tint.
However, it should be taken into account that the color of plaque can be affected by smoking, drinking and eating.
Disease prevention
Dental measures include:
- Regular thorough oral care.
A properly selected toothbrush, constant flossing, and rinsing your mouth after eating will help avoid inflammatory processes.
- Use a toothpaste that suits the purpose at this stage. You cannot use whitening or medicinal pastes constantly, only in courses.
General preventive measures:
- Healthy lifestyle
- To give up smoking
- Regular medical examinations
How is the treatment carried out?
Treatment for stomatitis is comprehensive.
- Anesthesia. To eliminate pain, the dentist may prescribe topical medications containing lidocaine or analgesics.
- Antiviral therapy. If the disease is caused by a herpes virus, the doctor prescribes antiviral drugs of the appropriate group of effects.
- Antibacterial therapy. In case of bacterial stomatitis, local treatment of the oral cavity with antiseptic solutions and dental ointments with antibacterial action is mandatory.
- Antifungal therapy. Stomatitis can be the result of fungal activity in the mouth. This form is more common in children, but is not excluded in adults. The specialist prescribes the patient a strict regimen of antifungal drugs.
- Anti-inflammatory therapy. It is carried out in cases of severe inflammation. The dentist recommends taking anti-inflammatory systemic drugs that have a targeted effect depending on the pathogen or cause of tongue stomatitis.
- Diet. Patients with stomatitis are prescribed a diet that excludes foods that can aggravate irritation of the mucous membrane and tongue. So dentists recommend avoiding hot, spicy, sour and salty foods. Smoking and drinking alcohol should be avoided.
Together with the treatment of stomatitis, treatment of diseases of the respiratory system, gastrointestinal tract, inflammation of the gums, caries, etc. can be carried out.
Expert opinion
Roman Borisovich Alekperov
orthopedic dentist
Experience: 24 years
Most often, red spots on the tongue are not accompanied by pain. A slight burning sensation or no symptoms at all creates a dangerous feeling that the problem will go away on its own. This can worsen the condition and cause serious consequences. If you have red spots on your tongue, consult a doctor. It is better to quickly take measures recommended by professionals than to spend a long time on treatment later.
Types of disease
Depending on the prevalence of the process and the predominance of a certain nature of changes, the following are distinguished:
Catarrhal glossitis
It is manifested by swelling, redness of the tongue, and the appearance of plaque on its surface, but the process does not extend to its deeper layers. Most often, catarrhal glossitis occurs with superficial injuries and burns of the tongue (chemical, thermal), oral candidiasis (disturbance of the balance of normal microflora), various forms of stomatitis, infectious diseases (viral and bacterial nature), as well as with a number of diseases (anemia, hypovitaminosis , metabolic disorders, diseases of the digestive system, etc.).
Ulcerative glossitis
It is usually manifested by the formation of single or multiple small ulcers on the tongue (the so-called aphthae, hence another name for it - aphthous glossitis). Ulcerations are often accompanied by bleeding, severe swelling, severe pain and deterioration in general condition. This type of glossitis can develop from catarrhal glossitis, and also be a manifestation of diseases of the oral cavity, gum diseases, and diseases of internal organs.
Purulent-phlegmous glossitis
It is a severe form of inflammation, spreading not only to the deeper layers of the tongue, but also to other tissues of the oral cavity; the nearby lymph nodes are also involved in the process. In this case, the patient’s condition is serious, with severe intoxication and elevated temperature, so such patients are usually treated promptly. Antibiotics for this glossitis are a mandatory component of treatment.
Where to contact
Any dentist will be able to help with advice, but it is still better to contact multidisciplinary clinics. The larger the clinic, the more patients, which means the doctors’ experience is much wider. In addition, high-quality specialists are rarely seen in modest dentistry on the outskirts of the city; they mostly work in large centers. Another reason to contact a multidisciplinary center is that they pay great attention to improving the qualifications of doctors, including in therapeutic dentistry.
The table shows contacts of 5 clinics where you will be advised about red spots on the tongue.
| Dental center | Clinic address | Working hours |
| ROOT | Moscow, st. Rustaveli, 14 building 9 8 800 775–26–37 | 10:00-22:00 seven days a week |
| Your smile.rf | Moscow, Palikha street, 10, building 9 8 | 9:00-21:00 seven days a week |
| Center Family Dentistry | Moscow, Orekhovy Boulevard, 59k2 8 | 9:00-21:00 seven days a week |
| Unident | Moscow, Bobrov lane, 4, building 1 8 | 9:00-21:00 seven days a week |
| CityDent | Moscow, st. Novocheremushkinskaya, 57 8 | 10:00-23:00 day off - Sunday |
Pain and burning of the tongue: how to treat?
Probably every gastroenterologist in his practice has encountered a patient with complaints of pain or burning of the tongue. Turning to this specialist in the first place is probably due to the following logical chain: the tongue is in the oral cavity, where the digestion process begins, which means that if a problem arises, you should visit a gastroenterologist. Old publications also come to the aid of patients and doctors of other specialties, in which chronic diseases of the digestive organs were considered as the causes of burning tongue.
But is it really that simple? Is pain and burning of the tongue a separate disease and who should treat it?
A little history and terminology.
Pain/burning in the tongue has many synonyms: glossalgia, glossodynia, stomatodynia, glossopyrosis, oral paresthesia, neurogenic glossitis, tongue neurosis, glossalgic syndrome. This condition is traditionally part of the so-called burning mouth syndrome or “burnt mouth syndrome,” in which pain/burning sensations are localized in various areas: tongue, upper palate, gums, lower lip, pharynx.
Burnt mouth syndrome (SMS) was first described back in 1880; in the 20th century, the term glossodynia, i.e., appeared. pain in the tongue, since unpleasant symptoms from the tongue were most common. This syndrome was first identified as a separate disease in 2004.
Almost all existing review articles and recommendations consider glossodynia within the framework of the SOP. General recommendations for the diagnosis and treatment of ROP may be applicable to the special case of glossodynia.
Definition
The International Association for the Study of Pain has designated glossodynia and oral burning as chronic pain, specifically “burning pain of the tongue or other mucous membranes of the mouth.”
Later, a detailed definition was given for ORS: “a burning sensation or sensation of altered sensitivity in the oral cavity, repeated daily for more than 2 hours a day for more than 3 months, without obvious causative lesions on clinical examination and examination.”
Epidemiology
Data on the prevalence of ROP and tongue pain/burning separately still vary from study to study. The average incidence of all cases of oral burning (including but not limited to tongue burning) is 0.1-3.7% of the population. Women suffer from this syndrome 2.5-7 times more often than men, especially often over the age of 60 and after menopause.
Common causes of pain and burning in the mouth.
There are two groups of reasons why patients notice a burning sensation in the mouth:
1) Primary (idiopathic), when there are no diseases of the oral cavity and other organs and systems, this will be the true SOR.
2) Secondary, caused by local (localized in the oral cavity) and systemic causes (autoimmune diseases, deficiency conditions, etc.)
Causes of secondary burning sensation in the mouth/burning tongue.
Possible causes of secondary burning sensation in the oral cavity are diverse and, oddly enough, are rarely associated with pathology of the digestive organs. A review published in 2022 on this problem identified the following conditions and diseases responsible for the occurrence of burning sensation in the mouth:
Local factors:
A. Diseases, conditions and damage to the oral cavity:
- fungal infection (eg candidiasis)
- lichen planus
- pemphigoid
- pemphigus
B. Trauma
1) Mechanical
2) Chemical
A. From the patient's side:
- toothpastes with abrasives
- use of mouth rinses with ethyl alcohol
- medications such as aspirin (applied to the sore tooth); over-the-counter medications containing phenols, peroxide, sulfuric acid
- vitamin C (citrus fruits)
- sour drinks
- lozenges and cough suppressants with high menthol content
b. From the dentist:
- Irrigation of the oral cavity with solutions containing methyl methacrylate, formaldehyde, formocresol, sodium hypochloride
- acrylic resin
- eugenol
3) Thermal: spicy or hot food or drink
C. Parafunctional habits
- Tongue sticking out, cheek biting, excessive tongue brushing
- mouth breathing
D. Xerostomia or impaired quality/quantity of saliva
- consequences of radiation or chemotherapy, Sjogren's syndrome, pathology of the salivary glands
- side effects of medications (antihistamines, antidepressants, diuretics, steroid hormones, non-steroidal anti-inflammatory drugs, amphetamines)
- smoking
E. Allergic reaction/contact hypersensitivity
- products, additives, flavors
- colorings and flavors from oral care products
- dental materials (nickel sulfate, cobalt, zinc)
System factors
A. Deficiency conditions: decreased levels of iron, zinc, folic acid, vitamins B1, B2, B6, B12
B. Endocrine pathology
- diabetes
- hypothyroidism
- hormonal disorders (changes in cortisol/sex hormone levels)
C. Autoimmune diseases
- Sjögren's syndrome
- lichenoid reactions
- systemic lupus erythematosus
D. Other diseases
- gastroesophageal reflux disease
- celiac disease
- multiple sclerosis
- Parkinson's disease
- Fabry disease
E. Medicines
- angiotensin-converting factor inhibitors
- antiretroviral therapy
F. Peripheral and central neuropathies
- diabetic polyneuropathy, neuropathy due to renal failure, neuropathy due to systemic connective tissue diseases, neuropathy due to HIV infection, postherpetic neuropathy, neuropathy due to chemotherapy
As can be seen from this huge list, most cases of burning of the tongue and in the oral cavity in general are caused by a dental problem/pathology, neurological, endocrine and autoimmune diseases. Gastroenterological causes (for example, gastroesophageal reflux disease) are rather the exception to the rule.
Primary burning sensation in the oral cavity (BOR) and its causes.
If there are no indications of secondary causes of burning in the oral cavity, most likely there is a true SOR. This is an independent disease, the cause of which is still unclear. In its development, the role of psychological factors and mental disorders, changes in the nerve endings and conductive nerve fibers of the oral cavity, as well as the central nervous system is assumed.
Clinical manifestations of ROP.
Symptoms that may bother patients with ROP are:
1) Pain and/or burning in the mouth of varying intensity. Some patients describe these sensations as tingling or irritation, as well as impaired sensitivity. The pain often occurs spontaneously, is often symmetrical and does not necessarily affect only one area. In the case of glossodynia, pain/burning is most often localized in the anterior 2/3 of the tongue, on its back, and lateral surfaces. The pain is minimal in the morning immediately after waking up, increasing in intensity throughout the day. Eating spicy, hot foods and drinks, as well as stress and fatigue increase the pain/burning sensation.
2) More than 70% of patients, in addition to pain/burning, note changes in taste, a decrease in its intensity, as well as the appearance of a foreign taste (bitter, metallic, or a combination of both). Most often, the sensation of sweet and salty tastes is reduced, and sour tastes are perceived more intensely.
3) Dry mouth (xerostomia) is noted by 46-67% of patients with SOP, while according to research data, an objective decrease in the amount of saliva is not observed in them.
4) Association with burning/pain from other mucous membranes has also been described in patients suffering from ROP. Most often this is a burning sensation in the rectum and genital tract. An alternative may be a feeling of dry mucous membranes (eyes, genital tract in women)
5) Night sleep disturbances are common (in 80% of cases) in people with SRS
6) Anxiety and depression are frequent companions of SOR and glossodynia separately. A meta-analysis of clinical studies showed that anxiety conditions increase the risk of developing RAS by 2.6 times, and depression by 3.2 times. Cancerophobia, social phobia, neuroticism, etc. are also often noted.
7) ODS is characterized by an association with other diseases that manifest as chronic pain: fibromyalgia, chronic back pain, chronic pelvic pain, irritable bowel syndrome, etc.
Treatment of SOR.
1) Patient information and support
Many patients with chronic oral burning and pain do not understand why their symptoms persist for so long. An important task of the doctor is to explain to patients with SRS the possible mechanisms of the formation of unpleasant sensations. Patients should be reassured that their symptoms are not imaginary or related to any form of cancer. This support will reduce anxiety, depression, fear and frustration, especially in individuals who have had previous unsuccessful treatment experiences.
2) Local therapy
Local use of clonazepam in the form of mouth rinses showed good results in reducing the severity of pain/burning in the mouth. There is encouraging evidence for the topical use of capsaicin (a chili pepper alkaloid) in low concentrations.
3) Systemic therapy
Tricyclic antidepressants, antidepressants from the group of serotonin and serotonin/norepinephrine reuptake inhibitors, clonazepam, and antiepileptic drugs (pregabalin and gabapentin) are actively used as drugs for the treatment of ORA. The use of alpha-lipoic acid has shown little effectiveness.
4) Non-drug psychotherapy
Given the frequent association of ODS with anxiety disorders, phobias and depression, non-pharmacological psychotherapy is an integral part of the treatment of this problem. Cognitive behavioral therapy, individual and group psychotherapy should be considered as methods of choice.
5) Physiotherapy and alternative treatments
Low-level laser therapy and acupuncture have been studied as methods for reducing pain. These methods were effective in some people with cerebral obstruction, but are not widely used.
Conclusion.
Identifying the causes of pain/burning in the oral cavity is a challenge for doctors of different specialties, but their friendly work allows us to solve the problem and improve the quality of life of patients.