Those who are familiar with severe lumbar pain or have serious problems with the spine know firsthand what a blockade is. This difficult procedure is considered today to be practically the only method of quickly relieving pain that arises in the back due to deformities or other pathologies of the vertebral arch. The blockade does not serve as a method of treatment and cannot be one. But an injection can relieve pain in a matter of minutes. What a blockade is, for what indications and how it is done, and what contraindications or complications this procedure may have is useful to know.
Blockade for lower back pain
Why blockade relieves pain
To understand the mechanism of action of the blockade, it is necessary to understand how pain occurs and how it affects.
Prices for painkillers for back pain
How pain occurs
Pathological phenomena in the spinal column are the reason why the spinal nerves become pinched. When a nerve is compressed, it transmits pain to a limb or neck, lower back, and so on. The location of pain depends directly on the location of the pinched nerve.
Pinched nerve in the lower back
Important! If the painful sensation occurs once or not often, it is relieved by a single dose of drugs that affect the source of pain. But if the symptom becomes chronic, a centralized inflamed pain focus forms in the cerebral cortex. It cannot be removed using standard treatment methods.
In cases where lower back pain becomes severe and constant, they resort to a blockade as the only way to relieve it. The injection turns off (disables) one of the links in the chain of movement of the pain reflex, which is why the entire movement of pain is interrupted, and the impulse does not reach the limbs and organs.
This procedure is not a method of treating back diseases, but only a way to relieve pain.
In some cases, a blockade injection is used for diagnostic measures to establish the true cause of pain.
Products for the treatment of injuries, muscle and joint pain
What is a blockade injection
What is this procedure? Through the injection, the nerve conduction of the fibers that transmit pain to the organs is reduced/switched off. For this purpose, local anesthetics are used, which act by inhibition to block sodium channels.
The pain syndrome goes away in almost a minute or two, and if this does not happen, a thorough diagnosis and search for other causes of pain are necessary.
For blockade, local anesthetics are used that block cell conduction by inhibiting voltage-gated sodium channels
The blockade injection is performed exclusively in the clinic, and only by doctors who have professional clearance for this procedure. A specialist needs not only medical knowledge, but also topographical and anatomical knowledge. Most often, specialists who meet the necessary requirements work in traumatology or neurosurgery in clinics and hospitals. Therefore, the procedure is carried out there.
Carrying out the blockade, photo
What is the difficulty of implementing a blockade? In the insecurity of the spinal cord. It would seem that, enclosed in a durable shell of the vertebral arch, the spinal cord remains one of the most vulnerable organs, which is afraid of the slightest penetration of bacteria. Viral infection of the spinal cord can lead to death of the patient. Therefore, the blockade is performed only under sterile conditions, where surgical operations are usually performed. The specialist wears gloves.
The procedure is carried out under sterile conditions
By the way. The procedure is reminiscent of taking puncture lumbar fluid, only during the blockade the patient is positioned differently, and the injection can be given not only in the lower back (depending on the location of the pain).
Advantages of blockade as an analgesic method
This method of relieving the patient of lower back pain has many advantages.
GV and anesthesia
The Association of Anaesthetists (UK) has published new recommendations on the use of anesthesia and sedation in breastfeeding mothers “Guideline on anaesthesia and sedation in breastfeedingwomen 2020” (Anaesthesia 2022, 75, 1482–1493). I will not write much about the arguments on various issues, but will simply give a short list of recommendations that should hang in the office of every obstetrician-gynecologist in the form of a large poster.
Women should be encouraged to breastfeed as usual after surgery.
There is no need to express and throw away breast milk.
Anesthetics and non-opioid pain medications pass into milk in excessively small quantities. For other drugs that are used during surgery, there is no reliable data on harm to the newborn.
Medicines like opioids and benzodiazepines should be used with caution, especially after multiple doses and in the presence of a baby under 6 weeks of age (adjusted for gestational age). In this situation, the newborn should be observed for abnormal somnolence and depressed breathing, especially in women who show signs of sedation.
Codeine should not be used by women who are breastfeeding due to the potential for excessive sedation in newborns due to differences in metabolism.
Any woman with a child under 2 years of age should be asked whether she is breastfeeding in preparation for surgery.
Non-opioid pain management techniques are preferred for hepatitis B. Local and regional anesthesia have advantages in this regard and have the least impact on a woman's ability to care for her baby.
If possible, day surgery (in day hospitals) is preferable so as not to disrupt the woman's routine activities. A woman having surgery as a day hospital is advised to have a responsible adult nearby for the first 24 hours after surgery. She should be careful about sleeping with the baby or sleeping in a chair while feeding the baby as she may not be as adequate as normal.
Breastfeeding support should be available to women undergoing surgery and medical procedures.
Patient information leaflets and additional resources should be available that provide information on the compatibility of anesthetics and analgesics during breastfeeding, as well as recommendations for perioperative breastfeeding support.
RETURN to Blog Dr. Elena Berezovskaya
Share link:
- Click to share on WhatsApp (Opens in new window)
- Click to share on Telegram (Opens in new window)
- Click here to share content on Facebook. (Opens in a new window)
- Click to share on Twitter (Opens in new window)
- Click to share on Skype (Opens in new window)
- Send this to a friend (Opens in new window)
- Click to print (Opens in new window)
By
What types of blockades are divided into?
There are many types of blockades. They are classified mainly by the location of the pain. But injections have not only a direct targeted effect. For example, a blockade in the neck, in the area of vertebrae 1-7, can relieve pain from the entire back, along the entire spine.
Table. Types of blockades by area of effect.
| Variety | Scope |
| It is done in the area of the six upper vertebrae belonging to the cervical segment and the seventh transitional segment. Relieves pain in the head and neck, and throughout the spine. Eliminates pain in the hands. |
| Thoracolumbar | It relieves pain in the lower back, legs, and also relieves pain in the intestines. |
| Blocks pain in the spine responsible for the lower back. |
| Combats pain at the lumbosacral level. It is often used (like the lumbar) for diagnostic purposes. |
| Level 1-12 thoracic vertebrae is the site of a thoracic blockade, which relieves pain syndromes in the upper extremities, torso, internal organs and throughout the back. |
| The difference between this type is that the injection is placed in a branch of the nerve without affecting the entire spinal cord. In this way, half of the body or a specific organ is anesthetized. This is enough to relieve narrow-point pain syndrome or perform a diagnostic procedure. An anesthetic substance is injected into the area of the paravertebral level (transverse vertebral processes). |
Blockades are also divided into types according to the point of administration and the drugs used.
The injection can be given:
- into the soft tissues surrounding the painful area of the spine;
- into biologically active segments of the muscular and ligamentous apparatus, as well as into tendons and active skin points;
- into nerve fibers;
- into nerve plexuses and nodules.
Depending on the drug used, injections are divided into:
- therapeutic (with the administration of a treatment drug, such as steroids);
- lidocaine (pain relief);
- novocaine (pain relief, diagnostics).
Injectable medications
Compositions for blockade injections are most often multicomponent. The main elements they contain are lidocaine and novocaine. These drugs are able to interrupt the process of nerve impulse transmission by inhibiting sodium passage.
ANESTHESIA FOR DENTAL TREATMENT
Local anesthesia in dentistry is designed to create comfort for the patient and the doctor. The patient gets rid of negative emotions, fear of treatment, and unnecessary shocks to the body. The doctor can work calmly, performing the necessary procedures according to the treatment plan.
Why do you need pain relief during dental treatment?
There are many times more nerve fibers in the tissues of the tooth than in the skin area; moreover, fibers with a high speed of pain conduction predominate in the tooth, so toothache is the most severe and unbearable. When treating teeth, it is very important for the doctor to properly anesthetize the teeth so as not to cause pain to the patient, as well as to eliminate unnecessary sudden movements during dental treatment caused by pain in the tooth, which can lead to a decrease in the quality of treatment or even breakage of the instrument. Many patients, fearing an injection, ask to have their teeth treated without anesthesia . However, the body's reaction is broader than just the painful sensations that the patient agrees to endure. Pain leads to a sharp release of adrenaline in the body, which causes an increase in heart rate, increased blood pressure, and increased sugar levels. Thus, anesthesia during dental treatment prevents the deterioration of the patient’s general condition. Painful sensations during dental treatment are well fixed in memory, and the next time we go to the dentist, our memory helpfully gives us the whole range of sensations, which already before treatment causes the release of adrenaline with all the ensuing consequences. Anesthesia during dental treatment reinforces the body’s normal reaction in memory and creates psychophysiological comfort.
Effect of drugs for local anesthesia in dentistry
Modern drugs for anesthesia in dentistry are produced in a convenient sterile form (carpules), which allows you to accurately administer the desired dose.
The action of the anesthetic is to block the conduction of nerve channels for some time. The duration of action of the anesthetic drug can be extended by using vasoconstrictor drugs several times, while the dose of the anesthetic itself does not increase. Refusal of pain relief during dental treatment only because of the fear of administering adrenaline is not justified; emotional stress will release more of it than the doctor will administer. Under stress, the body releases from 0.05 to 0.2 mg of adrenaline, and the drug for local anesthesia in dentistry contains several times less. There are contraindications for the use of the vasoconstrictor component - these are severe forms of hypertension, diabetes, arrhythmia, acute conditions after myocardial infarction, etc. Typically, such patients either postpone dental treatment or undergo hospital treatment based on the profile of the underlying disease. When using certain medications (beta-blockers, antidepressants, MAO inhibitors), it is necessary to inform the doctor before starting dental anesthesia , then the minimum dose of adrenaline is selected.
An important indicator of the safety of an anesthetic is its half-life - that is, the time during which half the dose of the incoming drug is eliminated from the body. Over six half-lives of the drug, its concentration in the blood plasma decreases by 98.5%.
Dental anesthesia during pregnancy
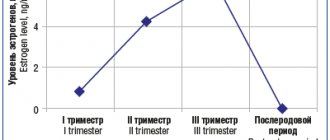
Dental treatment for pregnant women is usually carried out in the second trimester. In the first trimester, it is recommended to completely abandon any medications, since during this period the formation of organs in the child occurs, and in the last trimester the reflex excitability of the uterus increases.
Dental anesthesia during pregnancy is carried out using drugs that have the least effect on the fetus. Mepivacaine and bupivacaine are not used for dental anesthesia during pregnancy , as they easily penetrate the transplacental barrier and cause a slowdown in the fetal heart rate. Preference is given to 2% lidocaine in combination with a vasoconstrictor component with or without long-term treatment.
Dental anesthesia in nursing mothers
Drugs introduced into the body penetrate into mother's milk, so it is important to select the drug and feeding time so that the concentration of anesthetic in the milk is minimal. The main characteristic of a drug for dental anesthesia in nursing mothers will be its half-life - the time during which the concentration of the drug in the blood plasma is halved. The shorter the half-life of an anesthetic drug, the faster its concentration in the blood plasma and, consequently, in milk will decrease. Among modern drugs for anesthesia in dental treatment, the shortest half-life is 20 minutes. When using this drug, after 2 hours its concentration will decrease by 98.5%, which will be safe for feeding an infant.
Anesthesia for dental treatment for athletes
Before important competitions, athletes undergo a doping test. It should be remembered that articaine-type drugs give a positive doping test within a week after treatment.
Contraindications for the use of local anesthesia in dentistry
At the stage of compensation for various diseases, the use of local anesthesia in dentistry is safe in almost all patients.
For patients with diseases of the cardiovascular system (less than 6 months after myocardial infarction, severe forms of coronary artery disease, arterial hypertension with blood pressure more than 180/100) and decompensated forms of diseases of the endocrine system (diabetes mellitus, thyrotoxicosis, pheochromocytoma), dental treatment with anesthesia is carried out only in conditions hospital for the main disease.
Patients with allergies to medicinal substances used for dental anesthesia , as well as to their components, are treated only with the conclusion of an allergist, after testing for sensitivity to the drugs used in the clinic at an allergy clinic.
For patients taking antidepressants, MAO inhibitors, and beta-blockers, anesthesia for dental treatment is used after consultation with the attending physician who prescribed the above-mentioned drugs.
Based on materials from the website of the Family Dental Clinic, a participant in our Center’s affiliate program
Previous
Next
Is it possible to feed a child after dental anesthesia?
Fortunately for nursing mothers, many modern anesthetics either do not penetrate into breast milk at all, or even if they do get into it, their concentration is so minute that they do not have any harmful effect on the baby’s body and are quickly eliminated.
The main task of a woman who is breastfeeding is to inform him about her situation during a visit to the dentist and find out after what time the anesthesia chosen by him will “leave” the body.
As a rule, you can feed the baby three to five hours after applying the anesthetic. During the forced break, you should simply express milk, lightening the breasts and stimulating the production of a new portion. To prevent your baby from suffering from hunger, you should express the required amount of milk before visiting the dentist. Moreover, breastfeeding experts advise feeding the baby using a spoon or syringe (without a needle), but not through a nipple. This is necessary so that the baby does not refuse the breast, from which it is much more difficult to “extract” food than from a bottle. This recommendation is especially true for long-term treatment of the mother with antibiotics.